New to the Fast Tract Diet™ ? Click Here
Acid Reflux – Fats or Carbs?
Question:
I suffer from acid reflux and am confused by conflicting information regarding what food causes reflux. I read that “foods high in fat slow stomach emptying, increasing upward pressure on the lower esophageal sphincter and increasing the chances that food and acid will reflux upwards.” This goes against your theory of acid reflux, doesn’t it?
Answer:
This idea has been around for some time, but I truly believe that carbohydrates are the real culprit based on the evidence I present in the Fast Tract Digestion Heartburn book. In the book I list over 100 scientific journal references including a report by Penagini R., which states “It is concluded that, in the light of present evidence, there is no sound rationale for clinicians recommending that patients with GORD (European for GERD) follow a low-fat diet.” and this paper by Pehl, et.al states that there is no difference observed in reflux between a high and low fat meal if calories are the same. Additional evidence and studies are presented in my four-part article on acid reflux.
The most likely reason that fat has been blamed for acid reflux in my view is the connection between fatty foods and carbs. We think of french fries and other deep fried foods including fried chicken or fish as “fatty”, but they also contain lots of carbohydrate i.e., french fries are made from potatoes and fried chicken and fish are coated in wheat or corn-based flour.
Also, in terms of delayed stomach emptying, this recent study and others indicate that high fat diets actually accelerate gastric emptying. In this study, they showed that mouth-to-cecum transit time (MCTT) actually decreased with high fat meals. In other words, food is moving more quickly to the end of the small intestine with more fat. This should help prevent bacterial overgrowth in the small intestine and reduce, not increase acid reflux

FP on Parsnips
Question:
After three years of searching for an answer, it only took a day for my symptoms to improve on the Fast Tract Diet. A quick question regarding the app vs. the book for FP. Why would 80g of parsnips in the app be 9 FP but only 3 according to the book? If in doubt should there be more like this, should I follow the book or the app for other food items as well
Answer:
Great observation. While developing the expanded database of foods for the mobile app, I realized that the GI (glycemic index) for parsnips published on the University of Sidney website was 52 (https://www.glycemicindex.com/foodSearch.php).
This is significantly lower than the GI of 97 published in their original database and included in the book “The New Glucose Revolution”, which the FP calculation was based on in the Fast Tract Digestion books.
In other words, the FP value in the books is based on that older GI. I have reached out the U. Sidney concerning this discrepancy but have not received a response. Maybe if more people ask, they will provide an answer. The bottom line is this: until I resolve this issue, it makes sense to use the most conservative GI, which translates into a higher FP for parsnips.

Am I Getting Enough Carbohydrates?
Question:
I started the Fast Tract Diet for my LPR. Dairy and nuts in my diet tends to upset my stomatch even though I use enzymes. I work out 6x a week and am concerned that my carbohydrate intake is too low. Am I getting enough carbohydrates?
Answer:
Chewing well may help with nuts, and you can always cut back a bit on the amount as they do contain fiber. Also, limiting diary may help in the near term, and low lactose dairy with lactase may be added back gradually at a later date.
While there are essential amino acids (which make up protein) and essential fatty acids (which make up fat), there is no actual dietary requirement for carbohydrates. So I wouldn’t worry about getting enough carbohydrates. But adding more fat calories is important when cutting back on carbohydrates. There is also a metabolic adjustment period as your body begins preferentially burning fats in place of lost carbs. I recommend giving it a week or two making sure to increase fats, especially saturated fats.

Are Elemental Diet Drinks Gut Friendly?
Question:
I was not able to figure out how to calculate FP for “Unsweetened Vanilla Elemental Drink”. Can you help me with this?
Answer:
I took a look at the nutrition facts and ingredients. Though this product does not have a measured glycemic index (GI), the carbohydrate sources are 54 grams of cassava root (Tapioca) Maltodextrin (GI 100), and 7 grams of sugar which I assume is sucrose (updated GI 62).
I used the FP calculator to calculate each component which yields a final FP of 3 per serving. This is low in symptom potential. While this product is low in FP, some of the other Absorb Plus elemental drink mixes contain significant amounts of fructose and hence the FP values will be much higher.
Update May 24, 2016: @Katrina Crocker contacted me concerning a typo in the ingredients for the Unsweetened Vanilla Elemental Drink. There is actually no fructose added to the unsweetened version, so I updated my calculation for this product. Also, I had used a GI of 81 for tapioca for calculating the FP of the maltodextrin in this product, but since this product actually used pure maltrodextrin from tapioca, the GI for maltodextrin is assumed to be the same as glucose – 100.

Should I take apple cider vinegar for my GERD?
Question:
I have had GERD for 3 years and last year I was diagnosed with Fructose Malabsorption. I have taken apple cider vinegar (ACV) 30 minutes before every meal to facilitate acid production in my stomach, but I found that some insist that ACV should not be taken for fructose malabsorption because it has fructose in it. However, in the Fast Tract Diet app, ACV has 0 FP. Would you recommend drinking ACV?
Answer:
ACV contains very tiny amounts of fructose (well under 1/10 of a gram in a tablespoon). Other carbohydrates are also negligible. Therefore, ACV is assigned an FP value of zero.
If it helps you, there is little harm as long as you take a sip of water after to clear the esophagus. Also, most people with GERD have normal amounts of stomach acid (read “Does low stomach acid cause GERD?” in this article), so it might not be needed.
You can have your stomach acid tested via the Heidelberg capsule test or an equivalent endoscopic procedure. Lastly, many people are fructose intolerant but also have other intolerances (fiber, resistant starch, sugar alcohol and lactose). I recommend limiting all these carbohydrate types with the Fast Tract Diet until symptoms are gone. Then try adding one type of carbohydrate at a time to see how your body reacts.
Does the Fast Tract Diet cure SIBO?
Question:
If I do indeed suffer from small intestinal bacterial overgrowth (SIBO) for a non physical cause, can I expect that following the Fast Tract Diet may “cure” me of this condition? Or will it always recur whenever I do not adhere to the diet?
Answer:
Great question. As I discuss in the Fast Tract Digestion Heartburn and Fast Tract Digestion IBS books, there are many possible causes of SIBO. If you can identify and address the underlying cause, there is good reason to believe you will be able to “cure” SIBO or at least become less susceptible to flares or blooms of SIBO. An example is someone who is lactose intolerant. Once they take lactase enzyme with lactose-containing foods or avoid lactose, the problem is solved. SIBO (post infectious IBS) from having a gastrointestinal infection, tends to improve or resolve months to even years after the event.
In many cases however, SIBO reflects a new normal – decreased ability to process fermentable carbohydrates and increased sensitivity to fermentable carbohydrates. The best course of action in my view is to treat this by limiting these in your diet. In most cases diligence will pay off with decreased sensitivity, but you will likely always need to keep fermentable carbohydrates in check as well as incorporate pro-digesiton strategies outlined in the books into your routine. For individualied help including a root cause analysis, you can reach out to us here.

Sorbitol (a sugar alcohol) in Rapidol Express
Question:
I’m forced to take a reflux suppressant called Rapidol for my very bad reflux and LPR. But it contains sorbitol, a sugar alcohol which can cause fermentation. I can’t limit the medication until the reflux eases, but the medication itself could be causing more reflux. Any advice?
Answer:
I believe you are referring to Rapidol Express which contains the following active ingredients:
– Phycodol™, an Extract from Brown Algae (coats the stomach)
– Sodium Bicarbonate (antacid)
– Calcium Carbonate (antacid)
This product is certainly better than H2 blockers and PPIs, but as you pointed out, Rapidol Express contains sorbitol. It is a fermentable sugar alcohol and might be alright if you don’t take a lot.
Gaviscon Advanced also contains a raft forming ingredient, alginate and is a better choice in my view.
Once the diet fully kicks in, you shouldn’t need any medicine before long. For your full recovery:
- Stick with your appropriate FP goal daily
- Put gut friendly practices into action
- Identify and address any possible underlying causes
The Fast Tract Diet App is great for #1 and 2, and our consultation program can help you with all 3.
Are too many veggies not good for SIBO?
Question:
I’ve been on the Fast Tract Diet for almost 3 months and completely off my meds during the time. But it seems like I’m taking a step backward each time I eat too many veggies even though all veggies combined are no more than 10 Fermentation Potential (FP). Any though?
Answer:
I can understand your concern with not being able to eat more veggies at this moment, but it’s great to see the progress you have made – off meds and able to control your symptoms most of the time.
It’s important to remember that it only takes 30 grams (just over one ounce) of undigested carbohydrates for your gut bacteria to produce 10 liters of gas. Also, FP can build up due to slowly fermenting hard-to-digest carbohydrates from previous meals.
As you progress initially by keeping your FP points low, you will almost certainly improve your tolerance levels. But it takes time for some people. Keeping an eye out for hidden hard-to-digest carbohydrates and following the pro-digestion behavioral practices outlined in the Fast Tract Digestion book(s) will help.
The new Fast Tract Diet mobile app should also help, which has greatly increased the number of low FP food choices. The app will have the FP points for over 800 different foods, drinks, condiments, supplements, etc.
Which Fibers Don’t Ferment (Gut Friendly)?
Question:
Are there any fibers that don’t ferment? Which would you say are necessities if I were to isolate those in my diet and exclude the rest?
Answer:
All forms of dietary fiber are potentially fermentable, but the least fermentable is cellulose. Cellulose fiber is long chains of glucose molecules chemically bonded together. But the type of chemical bonding between the glucose molecules makes cellulose a tough fiber.
Cellulose is found in fruits, legumes, whole grains, and green vegetables. For most people, cellulose is a low risk fiber. The trouble is that many foods that contain cellulose also contain many other types of fiber, some of which are much more fermentable and more likely to invoke symptoms.
My advice is to consume low Fermentation Potential, FP vegetables, fruits and even some starches in moderation while limiting other higher FP choices.
Refer to the Fast Tract Digestion book(s) or soon to be released Fast Tract Diet app for help in choosing low FP foods.
Don’t High GI Foods Feed Bad Bacteria in Large Intestine?
Question:
I finished the Fast Tract Digestion book, great book. I like the theory behind it. I am wondering though if the foods with a high Glycemic Index (GI) would be feeding other bad organisms that may be present in the large intestine ?
Answer:
The answer is no as high GI carbohydrate-containing foods are easier to digest. Once they are fully digested, the single sugars from high GI carbohydrates are rapidly transported out of the intestine into the blood stream. This is also the reason that you should not overdue high GI carbohydrates (high blood sugar levels).
Low GI carbohydrates are broken down slowly and the sugars are more likely to feed potentially symptom-causing blooms of intestinal bacteria.
In cases where SIBO is extensive or extends to the early part of the small intestine, high GI carbohydrates could actually become part of the problem and a lower overall carbohydrate diet would be recommended in the short term, which allows your body to clear out the SIBO.
Both high and low GI carbohydrates are capable of feeding bad as well as good bacteria. It depends more on the metabolic capabilities of each type of bacteria. This really means whether they possess the enzymes to break down the various types of carbohydrate or not. But low GI carbohydrates are more available since they are not digested and absorbed as efficiently.
How Can I Convert Grams & Ounces to Common Household Measures for Foods in the FP Tables?
Question:
I appreciate the pre-calculated 16 FP food tables in the Fast Tract Digestion books that shows symptom potential in foods. But, they are in ounces and grams and need to be converted to ordinary household measures in order to know how much food we’re dealing with (teaspoon, tablespoon, cup, etc.) It requires buying a scale or visiting the grocery store and taking down all the label numbers for each product in which you’re interested. Is there an easier way to implement the diet?
Answer:
Thanks for the question.
Common household measures are available in the Fast Tract Diet mobile app for Android and iPhone/iPad. The mobile app complements the books including 800 foods / drinks (more than doubling the number of foods in the FP food tables) in common household measures and grams. The app will also have a meal and symptom tracker, FP calculator, shopping list, etc. You can calculate FP on your specific brand of foods and drinks on the fly.
The dashboard gives you a trend of your FP vs. symptom on a graph by week and month, so that you can monitor your progress. Best of all, the app will feature voice recognition.
Is Gellan Gum in Almond Milk Safe for SIBO?
Question:
I use the Trader Joe’s almond milk, but just noticed that it contains gellan gum and zanthan gum, both of which are not allowed on the Sibo diet. What is your view?
Answer:
Both gellan gum and zanthan gum are complex polysaccharides (chains of sugar molecules) that are produced by non-pathogenic bacteria. Since both are fermentable by gut bacteria, they are capable of producing GI symptoms if consumed in large amounts. The fermentation potential (3 grams for one cup) is quite low for unsweetened almond milk.
I’m not aware of any human safety issues with either gum, but in a rat study (not sure of the amount used, but likely much higher than product concentrations), the gellan gum groups exhibited a stickiness property that caused the intestinal microvilli to stick together. If this were to happen in people, you might imagine that your digestion would be much less efficient, potentially resulting in malabsorption and SIBO.
This may not be relevant with concentrations used in almond milk, but it’s hard to tell without comparing the quantity used in products with that used in the rat study and possibly conducting additional testing in humans. For making solutions more viscous, approximately 0.1 to 0.5 % is used. If you go over 1%, you typically create a gel.
If you consume almond milk regularly, perhaps you can make your own almond milk without any additives.
Is the Fast Tract Diet Effective for Gastritis?
Question:
I have been diagnoses with both gastritis and acid reflux. Is the Fast Tract Diet effective for gastritis just as it would be for most other GI conditions?
Answer:
Gastritis which means inflammation of the stomach is distinct from acid reflux and SIBO. And gastritis has many causes.
H. pylori is the most common cause, but over use of NSAIDs, alcohol abuse or an autoimmune condition called autoimmune metaplastic atrophic gastitis (AMAG) can also be involved. Gastritis may be acute or chronic. It can affect different areas of the stomach (cardia, body and antrum) and may be erosive or non-erosive in nature.
Successful treatment will depend on learning more about your specific condition and identifying and addressing the underlying cause(s). If you need help, consider our consultation program.
The Fast Tract Diet specifically targets SIBO and related conditions. Controlling bacterial overgrowth will reduce the amount of bile, bacteria and digestive enzymes being refluxed into the stomach and beyond. That may reduce irritation and improve gastritis in some cases, but this is speculative. I can’t guarantee the diet will resolve gastritis without taking the steps outlined above.
Are Gluten Free Flours Easy to Digest?
Question:
After rice flour made from jasmine rice, how would other gluten free flours rank as far as their symptom potential (i.e. Fermentation Potential, FP)? Any idea about the FP of tapioca flour, potato starch, sprouted oat flour and sprouted corn flour?
Answer:
Tapioca flour and potato starch both have relatively low FPs. ¼ cup of Tapioca flour has 4 FP points and the same amount of potato starch has 2 FP points.
Sprouted grains are reportedly easier to digest and should therefore have higher GI values and lower FP values. Unfortunately, I don’t have the specific FP for the sprouted oat and corn flour because there are no GI values available as far as I can tell.
One product that was tested for GI is sprouted 3 grain bread by Stonemill. The GI was measured as 55 giving an FP value of 7 for one slice, which is not terribly impressive and leading me to question the “easier to digest” claim. But someone on the Fast Tract Diet FB page indicated that these sprouted grain breads also contain un-sprouted flour which makes my conclusion questionable.
The bottom line is this. We need more research into the digestibility of sprouted grain products to make a final conclusion and determine accurate FP values for these grains.
One assumption you could make is that sprouted oat and corn flour should not be any worse than the corresponding non-sprouted grains.
– ¼ cup of oat flour consumed as porridge = 7 FP
– ¼ cup of corn starch = 4 FP
– ¼ cup of whole grain corn meal = 9 FP
Stay tuned for the Fast Tract Diet mobile app for Android and iOS coming out this fall. The app includes over 30 flours and grains out of 800 foods and drinks.
Is SIBO Autoimmune Disease?
Question:
What do you think about Pimentel’s theory that SIBO is actually autoimmune disease?
Answer:
This is fascinating research. They seem to be on to something for a subset of people with IBS – who previously experienced food poisoning (gastroenteritis) caused by certain bacterial pathogens that produce a toxin called cytolethal distending toxin B (cdt B). Antibodies to this toxin cross-react with other human proteins including a protein called vinulinwhich is involved in normal gut motility.
But there are many other IBS sufferers whose condition was brought about by other means including a variety of other motility disorders, digestive enzyme deficiencies (cystic fibrosis as the extreme example), antibiotic use, lactose or fructose intolerance or simply consuming more fermentable carbs than one’s body can process, particularly as we age. Each of these cases (and others) can lead to SIBO or general dysbiosis and IBS, GERD, leaky gut and other SIBO-related conditions.
Gut Microbes Feed or Impede?
Question:
Experts in this area (Sonnenburg – The Good Gut & Huffnagle – Probiotic Revolution, for example) tend to strongly emphasize the importance of high fiber, high resistant starch diets to maintain a healthy microbiota within the colon. Obviously they are not taking into account SIBO, but given the Fast Tract Diet is designed to deprive SIBO causing bacteria in the small intestine of their required fuel (fermentable carbohydrates), would this approach not also deprive the bacteria in the colon of the same fuel and lead to an unhealthy / unbalanced colonic microbiome?
Answer:
Good question and one I have thought about quite a bit. A simple answer is no and here is my answer in two parts.
The first part has to do with changes over the years in our microbiota. With rampant use of antibiotics and preservatives along with more cooked and processed foods, there is no doubt the diversity of our gut microbes has been reduced. This change could make it more difficult to process huge amounts of fermentable and complex carbohydrates as we may have once been able.
The second part has to do with how we count fermentable carbohydrates. The strict definition focuses on dietary fiber in its various forms. But I think the definition should be expanded to include all carbohydrates that routinely escape digestion / absorption and are available for fermentation. Thus I created the FP formula to measure this.
The number of fermentable carbohydrates is also higher for people with various carbohydrate intolerances (i.e. lactose, fructose intolerance, etc.) You can add fiber and resistant starch intolerance as well. In addition to fiber, other foods containing fructose, sucrose, lactose, resistant starch and sugar alcohols have many of the attributes of dietary fiber.
When you look at things in this way, we are not starving our gut microbes but more likely overfeeding them. The typical Western diet contains well over 100 grams of fermentable carbohydrates per day when you measure them using the Fermentation Potential (FP) calculation as explained in the Fast Tract Digestion books. The Fast Tract Diet recommends limiting FP under 45 grams a day. This is much higher than the 12 grams of dietary fiber per day cited by Sonnenburg and others. Over feeding our gut microbes can result in blooms of bacterial growth, SIBO and dysbiosis, but a less diverse microbe population overall.
Why Does The Fast Tract Diet Include Processed Foods?
Question:
I am a health conscious individual and was surprised to see that the food tables in the Fast Tract Digestion books include some processed foods. Although the Fast Tract Diet worked like magic, I am curious as to why you recommend processed foods.
Answer:
Let me be clear, I am not recommending that people eat processed foods. The food tables in the Fast Tract Digestion books and in the Fast Tract Diet mobile app on Android and iTunes list a large variety of whole foods including vegetables, fruits, starches, meat, seafood, etc. I personally practice a lower carbohydrate / not-so-strict paleo whole foods type diet based on controlling Fermentation Potential (FP), which includes seasonal vegetables from my own organic garden.
Please remember that the Fast Tract Diet is a flexible point system adaptable to a variety of dietary preferences and you are empowered to make your own food and drink choices as long as they are within the FP guidelines for relief from SIBO and related symptoms.
The Fast Tract Diet works on a similar principle as the Weight Watchers program, except that you monitor your FP points instead of calories.
There are two main reasons that some processed foods are included in the tables:
1. To show that some of them have high symptom potential and you should avoid or limit them.
2. They are commonly available in the market place and some people choose to consume them for convenience so we want these folks to have access to the FP points for those foods.
High GI Carbohydrates and Low FP Foods
Question:
I hear that low Glycemic Index (GI) foods are healthier because they do not raise blood sugar, but low symptom potential (i.e. fermentation potential – FP) foods in the Fast Tract Digestion books are high in GI. How do I reconcile the conflict in applying the Fast Tract Diet?
Answer:
I recognize that too many carbohydrates, particularly high GI carbohydrates can contribute to increases in blood sugar levels which can present problems for people with diabetes, other insulin-related or metabolic issues. But the best way to combat these issues is controlling the actual levels of dietary carbohydrate. This is by far superior to the low GI approach.
Low FP foods include both high carbohydrate, high GI foods as well as low carbohydrate foods. Using this combination of low FP foods allows one to address SIBO, IBS, GERD, LPR, etc. while controlling blood sugar at the same time.
The Fast Tract Diet described in the books recommends approximately 75 grams of carbohydrates per day. It is a lower carbohydrate diet compared to the 300 grams in the Standard American Diet. Depending on your individual tolerance for carbohydrates you can adjust the levels of carbohydrate in the Fast Tract Diet. Obviously, people with diabetes, metabolic disorders, etc. should adopt a lower carb diet.
Would Simethicone Reduce Gas?
Question:
Thanks for this great book! Would using simethicone be beneficial to reduce gas from SIBO?
Answer:
While the safety and side effect profile for simethicone appears to be fairly benign, this product does not reduce intestinal gas which is produced by intestinal bacteria. But if it breaks up some gas bubbles and works to help you with symptoms, I don’t see a huge downside.
My preference is to first employ dietary and behavioral strategies outlined in the Fast Tract Digestion books to control symptoms and improve gut health.
A Ten Year Old with SIBO
Question:
Can the Fast Tract Diet be used with a child aged 10 who has symptoms of SIBO?
Answer:
Of course, it’s always a good idea to discuss your child’s diet with your pediatrician. But since the Fast Tract Diet consists of healthy fats, carbohydrates and proteins from a variety of plant and animal sources, it should be absolutely fine for your 10 year old child.
It will also help reinforce good decision making on snack and junk foods as many are high in FP points and should be limited.
Supplements
Question:
Would you recommend people stay on any supplements they are currently taking when they start the Fast Tract Diet? I’m of two minds. Part of me thinks it might be tough to determine what’s actually helping, the diet or the supplements (or the combo!). But I’ll take whatever help I can get for symptom reduction.
Answer:
This is a great question but one that’s not black and white. In general, taking fewer supplements is best as many supplements have not been adequately studied for their safety and effectiveness.
As you mentioned, multiple interventions make it more difficult to figure out what’s helping or not. Also some supplements may actually impede progress or carry health risks. For instance, some probiotics can make bloating worse. People with adequate amounts of stomach acid could have worsening symptoms taking betaine HCl. Taking too much iron in the absence of a clear deficiency can cause serious side effects, even death.
On the other hand some supplements are helpful and don’t have much of a down side. For instance, lactase enzyme is safe and effective for treating dietary lactose intolerance.The same can be said for amylase enzyme to improve starch digestion. Basic vitamin and mineral supplementation is also a good idea with SIBO-related conditions as vitamin and mineral malabsorption is common in these cases.
Here are three things to consider when thinking about supplements:
1. Identifying the underlying cause of your symptoms is the best way to determine how diet can help and if supplementation is needed.
2. If there a clear need, choose a supplement that is safe and effective, and also backed by science.
3. Ensure that the supplement does not simply mask problem or cause additional side effects.
 Soy Protein Isolate Powders and Tempeh
Soy Protein Isolate Powders and Tempeh
Question:
I am a vegetarian looking for a low symptom potential (FP) protein source. Where would soy protein powder and tempeh be placed on the FP scale?
Answer:
Most soy protein isolate powders have low total carbohydrate and fiber counts, similar to whey protein isolates. The FP value is very low depending on the brand.
But, tempeh has a moderate FP, 13-14 for a single serving (113 g). I would lower the standard serving size for tempeh until your symptoms are improved.
Is Lactose Free Milk OK?
Question:
Thanks to the Fast Tract Diet! I am feeling much better just in a couple of days. Now that I am not drinking regular milk, I would like to find a substitute. I think lactose free milk is OK, isn’t?
Answer:
A cup of lactose free milk has a symptom potential (FP) of 5, so not too bad. The reason the FP value is not zero is because while lactose-free, it contains some fermentable oligosaccharide sugars.
There are other milk alternatives including rice, almond, coconut, and soy, etc. that are also low FP. Just make sure to choose unsweetened.
Erythritol (SIBO Safe Sweetener)
Question:
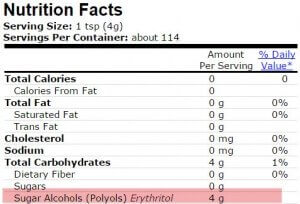
Erythritol is a seemingly safe sugar alcohol based on new information and I have seen a few different brands. The Swerve brand has oligosaccharides in the ingredients. Is this to be avoided? The Now brand lists only erythritol crystals… Would this be a better choice?
Answer:
I looked up the nutrition facts for Swerve. Though they mention that the product contains oligosaccharides, they don’t list the actual amount. If they did, you would count oligosaccharide content as dietary fiber in the FP calculation. I would avoid this product. The Now brand of pure erythritol is a better choice. You can also get erythritol blended with stevia.
For other SIBO safe sweeteners, refer to the Fast Tract Digestion books.
Jasmine Rice and Digestion
Question:
I tried Jasmine rice the other day, but it came out completely undigested. I am confused because Jasmine rice should be one of the legal foods in the Fast Tract Diet. Why was I not able to absorb/digest it? Do I need to supplement with amylase enzyme?
Answer:
Jasmine rice is the easiest starch to digest, so I share your concern. Here are some possible reasons that could lead to poor digestion of even easy-to-digest starches:
- Damage from small intestinal bacterial overgrowth, SIBO – as we have discussed in previous Q&As, people with SIBO often digest foods less efficiently than healthy people because of damage to the villi or microvilli digestive structures in the small intestine, as well as the enzymes on the microvilli.
- Deficiency in amylase enzyme needed to digest starch – the number of human amylase gene copies vary quite a bit from person to person. Your suggestion to try an amylase supplement makes sense.
- The rice not being prepared correctly – confirm that you ate freshly cooked Jasmine rice. If it was cooked, cooled and reheated, it could resist digestion/absorption due to an increase in resistant starch.
- Consuming more rice than one’s body is capable of digesting – if this was the case, reduce the serving size to ½ cup prepared rice.
I suggest you hold off on Jasmine rice until your symptoms improve. But, if you want to try again, make sure that you eat freshly made rice, chew well and eat slowly. This gives your amylase better access to the starch molecules and more time to act before food makes it to the acidic stomach destroying the amylase.
Coconut Yogurt and Symptom Potential (FP)
Question:
I am wondering if coconut yogurt has the same symptom potential (FP) as coconut milk. Being Paleo, coconut yogurt is a godsend.
Answer:
For one container (170 g) of Coconut Grove Plain Coconut Milk Yogurt, the FP is 8. Not too bad. This compares to the same serving size of regular plain milk-based yogurt which has an FP value of 6.
Millet and Symptom Potential (FP)
Question:
I see millet is not mentioned in the Fast Tract Digestion books. While thought of as a grain, it is actually a seed. It is deemed one of the world’s healthiest foods and I like to include it from time to time, although I’m enjoying the jasmine rice. So I’m wondering about its symptom potential (i.e. Fermentation Potential – FP).
Answer:
Great question. When prepared as porridge, 1/4 cup of raw hulled millet has an FP of 12 grams. However when millet flour is used to make flat bread, the FP is 1 gram per slice.
Fermentation Potential (FP) for Herbs
Question:
Are the fibers/carbs in powdered herbs anything to be concerned about in terms of fermentation potential? Not concerned so much for basil or other green culinary herbs, but more those made from roots or fruits, i.e. a teaspoon of, say, powdered cinnamon, or ginger, turmeric, curry powder or paprika?
Answer:
I have been recently studying the FP of herbs, so this question is timely.
Herbs range from 0 grams to 5 grams per tablespoon. Fresh herbs such as parsley, bay leaves and basil are on the low end (0-1), turmeric (2 g) in the middle with ground ginger (3 g), Paprika (3 g), curry powder (4 g), and ground cinnamon (5 g) on the higher end. A teaspoon has 1/3 the FP values listed above.
Do Fermented Foods Produce Gas?
Question:
I heard that fermented foods are good for digestion because they have less fermentable carbohydrates, but could already fermented food be re-fermented: therefore, producing gas in my intestines?
Answer:
Fermented foods are already fermented, though not quite to completion before you eat them. Unsweetened fermented foods (i.e. dill pickles, plain yogurt, etc.) in particular are much lower in fermentable carbs.
However, there are still some carbs in fermented foods. Plain yogurt still contains 4-6 grams of Fermentation Potential (FP) per cup depending on the brand. FP as you may know is symptom potential of foods you eat.
So yes, they could produce some gas, but not as much as the pre-fermented foods such as the milk used to make yogurt or the cucumbers used to make pickles. For more information on symptom potential of foods in FP points, refer to the Fast Tract Digestion book(s).
Does the Fast Tract Diet help with Bloating?
Question:
I have terrible bloating. Can the Fast Tract Diet help? If so, how?
Click here to learn more.
Food allergies and SIBO / IBS
Question:
Do you think food allergy testing is important for SIBO/IBS?
Click here to learn more.
Agave and Fermentation Potential
Question:
Is Organic Blue Agave sweetener acceptable?
Answer:
Great question. Agave nectar, also referred to as agave syrup is a high fructose sweetener. One teaspoon of agave (7 grams) contains 5.3 grams total carbohydrates, most of which is fructose. Agave’s Fermentation Potential (FP) is 5 points (grams). This FP value is high as its easy to consume more than one teaspoon of any sweetener.
Recall that gut bacteria can make 10 liters of gas from 30 grams of unabsorbed carbohydrate. That means that each teaspoon of agave (5 grams of unabsorbed sugar) can give rise to 1.6 liters of hydrogen gas. So I recommend caution with this sweetener.
For alternative low FP sweeteners, refer to the Fast Tract Digestion books.
Inulin and Fermentation Potential
Question:
What’s the status of inulin in the Fermentation Potential (FP) universe. I drink a lot of hot chicory beverage (Le roux). I wonder if it’s contributing to my SIBO distress.
Answer:
Inulin is a type of dietary fiber that many plants use (as an alternative to starch) to store energy in their roots or rhizomes (underground plant stems). Inulin is composed of chains or polymers of fructose and is not digestible by humans.
Inulin is considered a prebiotic potentially feeding healthy gut bacteria such as bifidobacteria and lactobacillus.
But this prebiotic property can also feed less desirable gas-producing bacteria resulting in gastrointestinal symptoms such as gas, bloating, cramps, etc. While some people can consume greater than 10 grams on inulin without side effects, many people will experience symptoms at much lower levels (https://jn.nutrition.org/content/129/7/1412S.full).
According the FP calculation used to measure hard-to-digest fermentable carbohydrates on the Fast Tract Diet, each gram of inulin equals one gram of fermentation potential.
Most chicory-containing drinks contain 1 to 3 grams of total carbs, but the exact amount of inulin is not generally listed. I recommend counting the total carb count from the nutrition label as dietary fiber in the FP calculation to be on the safe side. Personally, I have experienced acid reflux from consuming these drinks and avoid them.
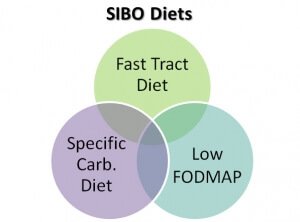
SIBO Diets
Question:
I am off of the elemental diet and reintroducing foods. I am trying to combine aspects of Specific Carbohydrate Diet, low FODMAP and Fast Tract Diet, but each diet is contradictory to each other. What would you suggest?
Answer:
Trying one specific diet at a time is the best way to go. Combining multiple approaches at the same time results in fewer food choices and potentially nutritional and caloric deficiencies.
If one diet doesn’t work after an adequate amount of time, stop and try another diet. At least with symptomatic GI conditions, you have a gauge to measure the success or lack of success on any diet or other approach.
While implementing the Fast Tract Diet, we can help you identify and address a variety of underlying causes and individual issues such as food intolerances, persistent symptoms, weight loss or weight gain through our consultation program.
For more information on the differences among 3 dietary approaches, refer to SIBO Diets and Digestive Health.
SIBO and Fecal Transplant
Question:
I have small intestinal bacterial overgrowth (SIBO) and would like to get rid of it once for all. Do you think that fecal microbiota transplantation (FMT) could be a cure for SIBO?
Click here to learn more.
 Bone Broth and Fermentation Potential
Bone Broth and Fermentation Potential
Question:
Is bone broth ok on the Fast Tract Diet? I do this mainly for my bone issues and it’s supposed to be very good for digestive issues.
Answer:
Absolutely. Bone broth is a gut-healthy delight. I will add bone broth to the soup section of the Fermentation Potential (FP) food table in the next book printing.
Depending upon the recipe, the FP of bone broth is either zero or really low. ENJOY!
Fruits and Fermentation Potential
Question:
I am a fruitaholic. I have a banana smoothie every morning, and usually snack between meals with fruit and use it as my night time treat mixed with yogurt. How do I best implement the Fast Tract Diet?
Answer:
While there are several low Fermentation Potential (FP) fruits, many fruits are higher in FP mostly due to fructose and fiber content, though bananas (especially if not fully ripe) also contain resistant starch.
Most people will need to limit fructose, fiber and starch-containing fruits to stay within the FP limits.
But not everyone is fructose intolerant. If you are one of those people (you can be tested), you may be able to tolerate more fruits. Also limiting does NOT mean eliminating. You can still have a few slices of ripe banana in your smoothie instead of the whole thing.
SIBO and Leaky Gut
Question:
Can small intestinal bacterial overgrowth (SIBO) cause leaky gut? If so, will the Fast Tract Diet help correct it?
Answer:
SIBO is most definitely linked to leaky gut, and the connection goes a long way to explain why SIBO is linked to many autoimmune conditions…Read more
Acid Reflux, LPR and Prescription Drugs
Question:
I am wondering why so many doctors are quick to prescribe proton pump inhibitors and H2 blockers, often both together for acid reflux and LPR. I’m worried about possible side effects from these medicines, especially if I need to be on them for a long time.
Answer:
This is one of the subjects that I am really passionate about, so my answer went beyond the usual scope of the Fast Tract Diet Q&A. Click here to read more.
Glycemic Index, Starch and Fat
Question:
I had a small serving of mashed potatoes as part of my dinner and experienced discomfort later on in the evening. The meal as a whole had a Fermentation Potential (FP) around 9 grams (chicken, small portion of zucchini, and mashed potatoes) which was within the Fast Tract Diet guidelines.
Since foods in combination have a different glycemic index (GI) than the individual foods taken separately (https://1.usa.gov/1Ez29Im), I am wondering how this affects the FP of the meal as a whole.
Answer:
I agree that mixed meals, especially when fat is involved, will affect the glycemic index (GI) of the whole meal. Still, you’re still better off choosing low FP foods if your goal is to keep FP low.
Also, here’s a little known fact. The GI lowering effect observed when starch and fat are cooked together involves “starch:lipid complex” formation. The complexes are harder to digest.
But these complexes are formed between amylose starch and fat. So high amylopectin starches, such as red potatoes or jasmine rice that are low in FP will be less subject to this effect.
Here are three suggestions:
1. Choose starches with the highest amylopectin to amylose ratio (lowest FP, refer to FTD Tables).
2. If you’re still concerned, consume a little less potatoes, make them fresh, eat slowly and chew well.
3. This suggestion is less appealing, but consume potatoes in isolation because most potatoes have some amylose in them.
Candida Overgrowth
Question:
I have successfully reduced SIBO to negligible levels, in part due to the Fast Tract diet. Thank you! The doctor indicates that candida is the chief problem now. Is the Fast Tract diet helpful for candida as well? I know candida is more yeast based and a different creature.
Answer:
SIBO has received a lot of press in recent years given its strong connection to IBS and so many other digestive (GI) and health conditions. But small intestinal fungal overgrowth (SIFO) can also result in GI symptoms as highlighted in this recent review.[1]
A variety of fungi including Candida albicans are natural members of our gut microbiota. For the most part, we never know they’re there. But unlike most fungi, C. albicans can overgrow under the certain conditions and even assume an invasive hyphal form that can cause tissue damage. [2] Read more
SIBO and Weight Loss
Question:
My main concern with SIBO right now is weight loss. How can I follow the Fast Tract Diet and gain some weight? I eat larger portions of the suggested menu.
Click here to learn more.
Ankylosing Spondilitis, Klebsiella pneumoniae and Fiber
Question:
I have been applying the principles of SIBO diet to my auto Immune Ankylosing Spondilitis (AS). I have dramatic results with NO starch, no dairy (without lactase), including going off all meds, reducing stiffness and pain most of the time.
When I have a relapse, I need to avoid ALL fiber (no vegies, no fruit, just protein foods and a very low fiber homemade strained juice). Somewhere I read that Klebsiella pneumoniae does not feed/grow on veggie fiber, however I have a hard time believing that. Can you shed some light on this?
Answer:
I agree, limiting starch, particularly amylose starch is a good strategy, but you should limit fiber as well. K. pneumonia can also degrade pectin, rafinose, stachyose, fructose oligosaccharide and other soy oligosaccharides. Here’s an old study.
Also, even if K. pneumonia could not use other forms of fiber, the breakdown of complex carbs is a collaborative activity where a wide variety of organisms – Clostridia, Bacteriodes, Klebsiella, Bifidobacteria, etc. work together to break apart these complex carbs and jointly use the partial or complete breakdown products.
Limiting overall carbs, particularly the hard-to-digest carbs (i.e. implementing the Fast Tract Diet) is the best way to reduce inflammation, leaky gut and overgrowth of gut bacteria including non desirable organisms such as K. pneumoniae.
SIBO Negative Reflux and IBS
Question:
I have reflux and IBS and take PPIs. I did a hydrogen breath test, but the result for SIBO was negative. You talk about SIBO being the cause of reflux and IBS. Does the Fast Tract Diet work for SIBO negative reflux and IBS?
Answer:
That’s a great question. SIBO, as you might imagine is always in a state of flux. Your body’s control mechanisms (stomach acid, efficient digestion of food, bile, immunity, motility, etc) are always working to keep intestinal bacteria in check, especially in the small intestine. But bacteria from the large intestine are often trying to work their way back into the small intestine where more nutrients are available.
I believe you can test negative yet still have periodic bouts or blooms of SIBO.
Other possible contributors to false negative results are:
1. Eliminating fiber and high residue foods from your diet well before the test. By doing this, you are actually beginning an intervention diet that helps control SIBO. I would like to see this practice adjusted to only limiting fiber the night before the test.
2. Using glucose instead of lactulose in the test. Glucose is absorbed very quickly and may not detect SIBO in some cases, but lactulose is not digested at all so can detect SIBO throughout the length of the small intestine.
My advice is to give the Fast Tract Diet a try. There is good reason to believe it will work for you.
Probiotics and Fermented Foods
Question:
I am taking Lactobacillus Plantarum probiotic supplement. Is this a good idea when having SIBO or would you recommend other strains of beneficial bacteria?
Answer:
According to one recent placebo-controlled study, L plantarum was associated with improvements in pain, bloating and feeling of complete evacuation.
Keep in mind, this study enrolled more vegetarian men and the same results might not be realized in Westerners on different diets. But the paper references some other studies that also show some benefits (see discussion section), although one smaller crossover study showed no benefit.
All in all, there is enough here in my view to give this probiotic a try. This probiotic is well tolerated. Another more natural way to get L. plantarum along with other lactobacilli is consuming kimchi, sauerkraut and other lacto-fermented veggies.
Quinoa and Fermentation Potential
Question:
I am a vegetarian with SIBO. I did not see quinoa listed in the Fast Tract Digestion (FTD) IBS book. Can you tell me the Fermentation Potential (FP) for quinoa?
Answer:
We will continued to add more foods in the FTD books when we update them. But, here is the quick answer. ¼ cup of dry quinoa (43 grams) has 14 FP points based on glycemic index of 35.
Note that the glycemic index was determined on cooked, cooled and microwave reheated quinoa. Freshly cooked quinoa would likely have a higher GI and hence, lower FP. But the bottom line is consume quinoa with a good degree of caution. If you do have some, make it fresh, limit the quantity to 1/2 cup, eat slowly and chew well. If you have symptoms, switch to a lower FP starch.
Klebsiella and Red Potatoes
Question:
In the Fast Tract Diet, red potatoes are considered low in symptom potential. But, they would fuel an overgrowth of Klebsiella, wouldn’t they?
Answer:
If the gut becomes leaky, Klebsiella pneumonia can stimulate antibodies that cross react with types I, III, and IV of collagen and HLA-B27 antigen through molecular mimicry in people susceptible to ankylosing spodylitis and rheumatoid arthritis. In these cases, limiting the growth of K. pneumonia is a good idea.
How to best accomplish this is the question. Avoiding all starch (and other carbs) is certainly the best dietary option. I have communicated with AS expert Dr. Alan Ebringer in UK extensively on this topic.
But the idea behind the Fast Tract Diet is that easier to digest amylopectin starch has a better chance of being fully digested and absorbed compared to amylose starch.
For that reason, low FP starches (with high glycemic indexes and higher amylopectin / amylose ratios) are preferred if you want to consume some starch in your diet. And red potatoes are more waxy, higher GI and lower amylose than other varieties. Of course, any starch that is malabsorbed can feed this bacterium.
One strategy is to omit all potatoes early on and then reintroduce low Fermentation Potential potatoes like red potatoes gradually being sure to follow the pro-digestion strategies discussed in the Fast Tract Digestion books.
 5 Hard-to-Digest Carbohydrates and SIBO
5 Hard-to-Digest Carbohydrates and SIBO
Question:
The Fast Tract Diet limits 5 hard-to-digest carbohydrates. Can some people tolerate some of these better than others or do we all need to avoid all five types?
Answer:
Yes, some people can tolerate some of these carbs better than others. Northern Europeans rarely experience lactose intolerance. They have evolved in this regard. Their lactase genes are stuck in the on position. Approximately 80% of the rest of the world remains lactose intolerant.
Also fructose intolerance, though prevalent, it is not a problem for everyone.
There is also variability in people’s ability to digest starch based on amylase gene (needed for starch-digesting amylase enzyme) copy number. People with more copies of this gene can digest starch better than someone with few copies.
Lastly fiber digestion depends on each person’s complement of fiber fermenting gut microbes.
Given all that, my strategy is to limit all five carb types using the Fermentation Potential (FP) point system to control SIBO and symptoms. When symptoms are under control, people can add each carb type back in a controlled manner, thus determining their specific intolerance profile.
Digestive enzymes including amylase, lactase and xylanase offer an additional tool to improve carbohydrate digestion.
SIBO, Elemental Diet and Fast Tract Diet
Question:
I have SIBO. My dietitian advised me to do the Elemental Diet, but I can not find good information on it. What is your view on the diet compared to the Fast Tract Diet?
Answer:
The elemental diet has been shown to be quite effective (80-85 percent cure rate) for people with SIBO because the only carbohydrate in elemental diet products is glucose which is easy to absorb and less likely to fuel SIBO.
Elemental diet products also contains predigested protein (free amino acids), and small amounts of fat in the form of easy-to-digest medium chain triglycerides. Lastly, the products contain essential minerals and vitamins.
But I would not recommend staying on the diet for more than two or three weeks as a whole foods diet is the healthiest in meeting our (complex) nutritional needs.
I recommend transitioning to the Fast Tract Diet after a couple of weeks. Keep in mind that full recovery depends on identifying and addressing any additional underlying factors that contributed to SIBO in the first place. The Fast Tract Digestion books and our consultation program can help with this process.
Red Potatoes and Symptom Potential
Question:
Re. the Desiree and Pontiac potatoes, they are red potatoes that are low in Fermentation Potential (FP) / symptom potential, but when I got to a store, none of the red potatoes are labeled. Are any red OK?
Answer:
While I can’t guarantee that all red potatoes will have the exact same FP, red potatoes are considered “waxy” meaning they have less amylose (hard to digest) and more amylopectin (easier to digest) starch.
I recommend trying the ones you have access to. Make sure you cook them well (baked is best), consume them fresh. Eat slowly, chew well, limit serving size and don’t consume leftovers.
Flatulence, Cause and Dietary Solution
Question:
I have had horrible flatulence for over two years. What could be the cause and how to fix it?
Answer:
Intestinal gas is produced by gut bacteria that ferment complex dietary carbohydrates and / or sugar alcohols as well as sulfur-containing amino acids from protein.
This could also be a sign of an imbalance in your gut microbiota or simply consuming too many complex carbohydrates.
The Fast Tract Diet should address this issue effectively because it is specifically focused on reducing excessive fermentation and the gas that goes along with it.
Inulin and Inulin Containing Supplements
Question:
Regarding the inulin in the products on gutsense.org, I am wondering if it is okay or must all people with reflux avoid all inulin.
Answer:
Great question. Inulin, a prebiotic dietary fiber from plants such as chicory root, is not digested or absorbed. But it is fermented by gut bacteria.
As you know, I recommend limiting the fermentable carbs for people with IBS, GERD or other SIBO-related conditions. This supplement is no exception.
Though inulin, like lactulose may have mild laxative effects, the side effects (bloating, gas, belching, flatulence, reflux, cramps, etc.) are not worth the benefit.
I was looking at the supplements on the Gutsense page and notice that some (Ageless GI Recovery for instance) contain inulin, but the amount is very tiny – only 250 mg or 1/4 of a gram. This amount is very unlikely to cause any significant unwanted GI reactions.
If you are following the Fast Tract Diet and your daily FP points were 35 grams, taking this supplement twice a day would increase your FP points to 35.5 grams. No biggie.
“Fermentable Carbs” vs. “Fermented” Foods
Question:
What are the differences between fermentable carbohydrates vs. fermented foods? I am a bit confused.
Click here to learn more.
Fermented foods and its benefits for digestive health
Question:
I have been hearing that fermented foods are good for digestion. Can you explain why?
Answer:
Fermented foods include yogurt, kefir, cheese, pickles, sauerkraut and other vegetables. The bacteria that drive the fermentation process are mostly lactic acid bacteria, though other types of bacteria can be used, for instance Bacillus subtilis for natto from soy beans and even molds, for instance for tempeh from soybeans.
Since fermented foods have already been fermented in the pickle or sauerkraut jar or yogurt culture etc., they are lower in carbohydrates and higher in short chain fatty acids (SCFAs), mostly lactic acid.
Here are some potential benefits from consuming fermented foods:
1. Fermented foods are low Fermentation Potential (FP). They have few remaining fermentable carbs so you can expect fewer symptoms such as bloating, cramps, altered bowel habits, reflux, etc.
2. Fermented foods contain lactic acid, butyrate and other SCFAs which are healthy fats our body can utilize for energy.
3. Fermented foods still contain many nutrients including vitamins – early American settlers depended on fermented foods to survive the winters.
4. SCFAs are acidic which is beneficial for our small intestine. Lactic acid is a natural preservative that bacteria in our small intestine also produce which helps ward off bad bacteria. Note: Acidic SCFAs also helps to extend the shelf life of fermented foods.
5. Fermented foods include some of the same species of bacteria that live in our intestines, especially small intestines. These bacteria can fortify our existing healthy small intestinal microbiota and help compete with bad or pathogenic bacteria.
6. Fermented diary helps with lactose intolerance because the bacteria produce the enzyme lactase.
Rice Mike and Fermentation Potential
Question:
I can’t eat soy, how about rice milk? Is it gut friendly?
Answer:
Rice milk is a gut friendly choice having relatively few Fermentation Potential (FP) points. I would suggest unsweetened because it is easier to digest compared to the varieties with sugar added. You can add your choice of low FP sweetener if needed.
Here are the Fermentation Potential (FP) points based on the FP calculation:
- Rice Dream Unsweetened Rice Milk (per cup):
FP: 1 - Rice Dream Original Rice milk (per cup):
FP: 2 - Australia’s own natural rice milk (per cup):
FP: 3 - Vitasoy rice milk (per cup):
FP: 5
Thanks to all our readers for the continued questions and feedback, we continue to add more foods and beverages to be included in new editions of Fast Tract Diet books and a new Fast Tract Diet Implementation Guide due out this summer as well as a Fast Tract Diet mobile app due out this fall.
 Cooked vs. raw veggies
Cooked vs. raw veggies
Question:
Is there a big difference in Fermentation Potential points (i.e. symptom potential) between cooked vs. raw vegetables?
Answer:
I don’t think it matters that much for lower carbohydrate veggies. For example cooked vs. raw carrots, the difference is only a couple of Fermentation Potential (FP) points as listed in the books, which indicates symptom potential.
But, it does matter for starchy vegetables such as peas, corn, plantains, grains, most root vegetables, and tubers. These have to be cooked really well to aid digestion.
If you do notice that certain raw veggies give you problems, I recommend either switching to cooked veggies, or reducing serving size.
 Constipation, SIBO and Methane
Constipation, SIBO and Methane
Question:
I suffer from chronic constipation and recently tested positive for methane by breath test. What does methane have to do with constipation and do you think the Fast Tract Diet will help?
Click here to learn more.
 GERD, H. pylori and Low Stomach Acid
GERD, H. pylori and Low Stomach Acid
Question:
Since I was diagnosed with GERD, I started reading a lot about it. What is your view on H. pylori & Low Stomach Acid being the cause?
Answer:
This is an interesting question. I also wondered about this myself and dug into it.
H. pylori and low stomach acid are not a common cause of acid reflux, but may contribute to something called atypical non-acid reflux in some people. This article has the details.
 Splenda and SIBO
Splenda and SIBO
Question:
I don’t like Splenda because it’s not natural and I have SIBO. This study suggests a negative effect on gut bacteria. What is your view?
Answer:
I totally respect your view. The Fast Tract Digestion books also suggest several natural alternatives to sugar including stevia for instance.
The most important thing for SIBO is to limit fermentable carbohydrates in your diet which include sucrose (i.e. sugar which contains fructose) and fructose (i.e. fruit sugar) itself.
As for the study, I view these results with a pretty big grain of salt for the following reasons:
1. The study was paid for by the sugar industry (who doesn’t like competition)
2. It was done in rats (is it relevant in humans?)
3. It has conflicting data (lack of a dose response)
Also, the study was discredited by an expert panel of scientists which concluded that “The study conclusions are not consistent with published literature and not supported by the data presented.”
At the end of the day, science is the judge. I continue to monitor studies on Splenda and other sweeteners and will post on these as they are published.
Jasm ine rice and Fermentation Potential
ine rice and Fermentation Potential
Question:
There are two kinds of Jasmine rice, brown and white. Which one would you recommend?
Answer:
I recommend white jasmine rice because the Fermentation Potential (FP) points are very low.
About brown jasmine rice, the FP is unknown because glycemic index data is not available as far as I know, which makes difficult to derive its FP points.
But, because brown rice is less processed in general, fibrous carbohydrates (bran and germ layers) will impede digestion over white jasmine rice.
 FP Calculator and Glycemic Index
FP Calculator and Glycemic Index
Question:
I want to use the free online FP calculator, but can not find Glycemic Index (GI) for the food I am interested in. What would you suggest?
Answer:
Here are a couple of websites where you can look up GI values: Mendosa.com and The University of Sydney website.
Though GI values exist for approximately 3000 different foods, many are culturally specific. Unfortunately, a GI value is not available for every single food in the market place.
The reasons being:
1. There are so many foods to test.
2. The test is expensive as it requires extensive testing on 10 people.
3. Testing of some lower carbohydrate foods is difficult because the test subjects must ingest a serving size with 50 grams net carbs.
If you can’t find a GI value, I recommend plugging in an average GI value of 50 for an estimate of the FP. For lower carb foods, the GI doesn’t actually matter that much and higher carb foods generally have been tested for GI.
The Fast Tract Digestion books list the Fermentation Potential (FP) or symptom potential for over 350 common foods including 60 vegetables. The books also give daily allowances of FP as part of a complete dietary solution. The Fast Tract Diet mobile app is another great resource, which has greatly increased the number of low FP food choices and included meal planning, point and symptoms tracking, voice recognition to look up foods on the fly and a built in FP calculator
 IBS and Gut Microbiota
IBS and Gut Microbiota
Question:
The Fast Tract Diet seems to starve all types (good & bad) of gut bacteria for my IBS. The ultimate goal to re-balance the microbiota is to use fermented foods and sometimes even antibiotics and antifungals, isn’t it?
Answer:
The diet does not “starve” gut bacteria. The diet limits (not eliminates) hard-to-digest fermentable carbs that feed gut bacteria. Gut bacteria are also fed by fermentable animal-based foods as well as fermentable mucus carbohydrate side chains that our own body produces.
People with IBS have been shown to have less diverse gut bacteria with an overabundance of gas-producing carb-loving firmucutes bacteria. In other words, too many fermentable carbs can actually decrease the diversity of your gut microbiota.
Another way to dramatically disrupt the microbiota is taking antibiotics which do not discriminate between healthy and unhealthy gut bacteria. Seems we have quite different views on this subject.
This diet strikes at the underlying imbalance not just the symptoms. The Fast Tract Digestion IBS book also dedicates an important chapter to evaluation and correction of other potential underlying contributing causes.
I believe the single most important underlying cause of IBS in most people is the modern Western diet.
 SIBO and Resistant Starch
SIBO and Resistant Starch
Question:
Can you comment on resistant starch? I have been on the Paleo diet and I learned that resistant starch should be helping small intestinal bacterial overgrowth (SIBO).
Click here to learn more.
 Honey
Honey
Question:
How come honey which is high in fructose is allowed on the Fast Tract Diet (FTD)?
Answer:
The FTD actually recommends limiting fructose-containing foods including sucrose, honey and maple syrup. But technically no food is illegal.
It’s all about counting the Fermentation Potential (FP) grams for the serving sizes of any food and making sure the overall FP points are within the limits for individual meals and overall daily totals.
For example, if you have one teaspoon of honey in your tea, you will add relatively a small amount of FP. Not too bad, but it can add up if you use too much.
 SIBO Diets and Half and Half
SIBO Diets and Half and Half
Question: Most diets for SIBO say don’t eat milk products. If I take half and half in tea with a lactase pill, am I going to be OK?
Answer: Yes, you should be fine. But milk and milk products also contain several oligosaccharides that behave as dietary fiber, which can be problematic in higher quantities. Therefore even lactose-free products still have fermentation potential (FP).
But since only a small amount of half and half is needed for tea, the FP value would be fairly low, particularly if you take a lactase pill.
 Psyllium Husk and IBS / SIBO
Psyllium Husk and IBS / SIBO
Question:
What is your opinion on taking psyllium husk for my IBS / SIBO?
Answer:
Above what you get from green stalked and leafy vegetables, I don’t think fiber is needed. In many people, fiber supplements make symptoms worse.
Also, some fiber supplements contain lots of sugar which is half fructose. Symptomatic fructose intolerance is very common.
Lastly the FDA has warned of choking and intestinal blockage risks associated with fiber supplements. I don’t recommend these supplements, but if you try them, experiment with small amounts and drink lots of water.
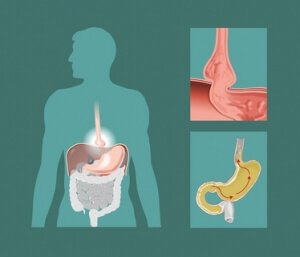 GERD with Hiatal Hernia
GERD with Hiatal Hernia
Question:
Does the Fast Tract Diet work for GERD with hiatal hernia?
Answer:
Having a hiatal hernia is a bit like wearing tight clothes or being pregnant. Because the hernia is essentially the top part of your stomach being pinched above the diaphragm.
There is often extra intragastric pressure (pressure in your stomach) that can trigger reflux. The Fast Tract Diet (FTD) is designed to reduce this intragastric pressure at the source, gas produced by overgrowing bacteria in your intestines which is fed mostly by unabsorbed carbohydrates.
There is every reason to believe that the FTD will help even in the presence of the hernia, but you might have to be extra diligent reducing FP points even more and following the proabsorption behaviors in the Fast Tract Digestion Heartburn book.
 Pregnancy and GERD
Pregnancy and GERD
Question:
I am 9 weeks pregnant and having a terrible time with GERD. Is the Fast Tract Diet safe?
Answer:
The Fast Tract Diet (FTD) is based on whole healthy foods and is fine for pregnancy. I am aware that gestational diabetes can arise half way into pregnancy sometimes. But, that is not an issue with FTD as the daily carbohydrate count of its meal plans is approximately 75 grams per day.
GERD and Asthma
Question:
The Fast Tract Diet helped my GERD and asthmatic symptoms. Why does the diet work for asthma?
Click here to learn more.
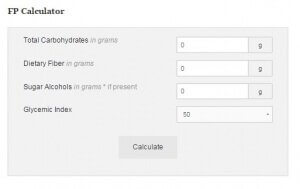 Fermentation Potential (FP) and FP Calculator
Fermentation Potential (FP) and FP Calculator
Question:
What is Fermentation Potential (FP) in the Fast Tract Diet and how does it work?
Answer:
FP is a mathematical formula that measures the symptom potential of foods. High FP foods are more likely to drive small intestinal bacterial overgrowth (SIBO) and other SIBO related conditions including acid reflux, gastroesophageal reflux disease (GERD), laryngopharyngeal Reflux Disease (LPR) and irritable bowel syndrome (IBS).
The Fast Tract Diet is based on the idea that certain carbohydrates are difficult digest because of their molecular structures in food chemistry. Difficult-to-digest carbs are more subject to malabsorption (a failure to be fully absorbed from the gastrointestinal tract). And they tend to persist in the small intestine, which potentially feeds blooms of SIBO.
Unless you are a nutritionist, it’s hard to know what types of carbohydrates are in each food and how much. The Fast Tract Diet solved this problem with FP. Give the free online FP calculator a try to see how it works
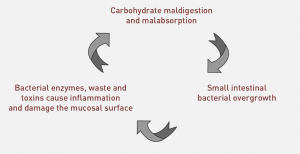 Specific Carbohydrate Diet
Specific Carbohydrate Diet
Question:
In the book, Breaking the vicious cycle, apple and banana are listed as legal foods. What is your view?
Answer:
Breaking the Vicious Cycle (Specific Carbohydrate Diet, SCD) is a groundbreaking book that helped bring to light the connection between diet and gut microbes in digestive health.
That being said, the SCD does not limit fructose or fiber consumption, but the Fast Tract Diet (FTD) does. Both apples and bananas have high Fermentation Potentials (FP) because of fructose in both fruits, and also resistant starch (up to 37%) in the case of bananas. Therefore, they have significant symptom potential.
You can still consume apples and bananas on FTD, but adjust the amount. For instance, start with one quarter of an apple or 1/3 of a ripened banana once your symptoms are under control. For more info. on the difference between SCD and FTD, refer to my blog article on SIBO Diets.
Calories
Question:
I feel hungry being on the Fast Tract Diet. What do you suggest?
Answer:
The diet reduces fermentable carbohydrates: therefore, you need to replace calories with low fermentation potential (FP) foods, proteins and fats.
Fats are not the enemy if you are concerned. These are a couple of readings for your reference.
Study: Doubling Saturated Fat in Diet Does not Increase Saturated Fat in Blood
 Fiber
Fiber
Question:
I am a little concerned about the lack of fiber for long term in the Fast Tract Diet, especially for my constipation. Thoughts?
Answer:
There is much more fermentable material (both from plants and animals) in our diet than we realize.
30-45 grams of fermentable carbs (FP points) per day is plenty to keep our microbes happy but not enough to make those of us with lower tolerance ill.
Unfortunately, the many health claims on dietary fiber are not supported by current research. And the dark side for digestive health is real.
As for constipation, a recent study reported that stopping or reducing dietary fiber intake actually reduced constipation.
 FODMAPs vs. Fast Tract Diet
FODMAPs vs. Fast Tract Diet
Question:
I want to try the Fast Tract Diet, but I have grown so confused dealing with all of the conflicting food advice. FODMAPs suggests avoiding onions, garlic, artichokes, asparagus, avocado, beets, broccoli, green beans, mushrooms yogurt etc.
Answer:
The FODMAP diet is an elimination diet. But, the Fast Tract Diet uses a quantitative approach based on Fermentation Potential (FP). For this reason, reasonable sized servings of vegetables that contain small amounts of FODMAPs are still acceptable as long as you keep your overall FP levels in line with recommendations.
For example, a few small cloves of garlic do contain a FODMAP (fructose oligosaccharide) but only a couple of grams which is also reflected in the FP value. So by following the low FP approach, you are also controlling FODMAP levels, but in a quantitative manner as opposed to just eliminating any food with even a trace of FODMAPs.




































Can you drink bone broth on a SIBO diet? I do this mainly for my bone issues and its suppose to be very good for digestive issues.
Absolutely sandp1. Such a gut-healthy delight. I should add a recipe and also add bone broth to the soup table in the book. The FP of bone broth is zero.
Cracked wheat (bulgar) is shown as having low fermentation potential. I am puzzled by that since whole grains and foods containing wheat in general are to be avoided or severely limited on the fast track diet. Would you please explain? Thanks.
Hi Susan, Thanks for pointing this out. There is a typo in the print book for cracked wheat. This has been corrected in the mobile app (I will correct the print book at the next print run). The app correctly lists (for a 1/4 cup weighing 40 grams) a GI of 48, total carbs of 29 grams, fiber of 5 grams and total FP = 17 grams.
Thank you for writing the book ‘The Fast Tract IBS’.
I have been on SCD, GAPS, FODMAP, also antibiotic treatments for SIBO with the result of still having SIBO. I am very excited with the information in your book because it gives me hope that I can still improve. With the gastroenterologist and dietitian I am also trying to figure out the underlying cause(s).
A few questions.
– Can mercury intoxication from amalgam fillings also cause SIBO?
– Can I take ‘Chlorella’ when having SIBO, on SCD diet Chlorella is not allowed.
– What is the FP of quinoa? couldn’t find that in your book.
– Can SIBO cause ‘Leaky gut’?
Thank you so much!
Kind regards,
Sofie
I wish Norm or someone in his office could address more of these questions!
Hi Norm,
I am taking Lactobacillus Plantarum probiotic supplement. Is this a good idea when having SIBO or would you recommend other strains of beneficial bacteria?
Thank you ,
Sofie
Hi Norm,
I have been reading a lot about biofilms & SIBO. I would appreciate your opinion on biofilms. I have your book, and it has helped me immensely. It makes perfect sense to that diet is the key and to limit the food supply that these “buggers” feed on.
Diet aside…….it is my understanding that SIBO is hard to treat with antibiotics & herbals as the “bad bacteria” protect themselves in a biofilm. The SIBO returns very quickly because the “bad bacteria” never really died off……the treatment did not break the protective biofilm. “Interfase Plus” claims to be able to break biofilms.
Can biofilms ever be penetrated and/or eradicated?…..or are they just hiding & waiting for the next opportunity to come out & feed! It seems that the Fast Track Diet will starve them to death. But is that true?
Thanks!
Joe
I’m also interested in this question, but see its not yet answered. I was planning on oredering a biofilm disruptor and herbal ‘antibiotic’ protocol for my daughter , but am concerned about die-off reactions especially as she’s very underweight. Should she just gain weight on the fast track diet before adding in these?
Thanks.
Thanks also Norm for your book and really helpful website.
Alison
Hi Norm,
Would the amount of sugar alcohols in sugar fee gum, such as Dentine Ice cause a problem? Chewing gum seems to help my GERD and satisfys my sweet tooth.
Thanks for all you do,
Jill
Hi Jill. Typically 2 grams per stick which can add up depending on how much you chew. The FP grams for sugar sweetened gum is about half that.
I’m a huge fan of your fast tract heartburn book and have coincidentally recently attempted again to go off my Rx PPIs, hopefully for good. I have been on and off the drugs for 4 years. Last year I had many bacterial infections and when on antibiotics nine times, which then resulted in thrush more recently. Now, my goal is to stay off the PPIs and recolonize my digestive tract with several strains of bacteria that are helpful for digestion in hopes of staving off my GERD. Any advice on probiotics here is most appreciated. Thank you so much.
Hi Elise,
Here is a comment I made on the Fast Tract Diet (Official) FB discussion group. You should join the conversation.
When you absolutely need to take antibiotics, taking a probiotic (needs to be resistant to the antibiotic in question) is an option some advocate. I am not aware of data showing their effectiveness, but maybe someone else can find some.
The biggest problem is that current probiotics don’t represent the incredibly diverse microbiota that is being decimated. Luckily, though perhaps not perfect, gut microbes do gradually repopulate over time. You are basically receiving a slow fecal transplant from other people and the environment. Unfortunately it can take months and may never restore the full complement you had to begin with.
Lastly, fecal transplantation research offers some hope for the future if things get really out of wack.
Hi Norm, Thanks for your book! I downloaded it the other day and really enjoyed it. I’m hoping it will help relieve my SIBO symptoms. I have a quick question…I realize that the FP for each food is around 35 for the first couple of week, but I was wondering what the average total carbs per day are on the Fast Tract Diet? I’ve been working with a nutrition consultant for fat loss and I’m trying to figure out if I can keep to my current macros and also do the Fast Tract Diet. Thanks!
Perfect Elizabeth. If you go by the recipes, they averaged approximately 75 grams per day. But some people consume less and some more depending on how complicated the SIBO is an other dietary preferences. Please keep us posted on your progress.
Hi Norm, and thanks so much for being willing to answer questions! I see people have already asked a couple that I wanted to know about (quinoa and psyllium).
I’m just reading your book and am about to go on the diet (for heartburn, which started recently with an oesophageal spasm, out of nowhere).
I had been taking resistant starch for some months and getting some good improvement in orthostatic intolerance (part of my ME/CFS) and am worried that I’ll lose that now if I stop (but I don’t think I’ve got much choice!).
I’m assuming I’d been helping to restore some sort of balance in my gut flora. Are all prebiotics off the menu? Someone suggested beetroot extract to me as an alternative to begin with that wouldn’t get me into trouble but I’m wondering if all prebiotics act through fermentation – but presumably it’s the amount of fermentation that’s the issue?
Hi Norm – another question!
I live in the UK so have access to different food brands than you have in the US.
Is there an easy way to tell what is a low-amylose rice cake? If I have to contact the manufacturer to find out, what should I ask them?
Thank you!
Oh – I’ve just realised that what you mean by ‘rice cake’ is probably something you get in a Japanese restaurant and that a ‘puffed rice cake’ is what we can get in the UK (a bit like polystyrene!).
Norm,
I soak all my nuts & seeds and dehydrate. I soak ALL grains & flours before I use to help reduce the phytates that are on them. I was diagnosed with nutcracker esophagus in 2008 and Barret’s non-dysplasia in 2014. My functional med doctor thinks it has alot to do with my histame issues I have (we are treating with maganese & molybelendum)which is helping. I feel somtimes I can’t eat anything anymore and can’t afford to loose weight. I do have a small hiatal hernia also. I also drink my own bone broth which not sure if good idea with histame issues.
Thoughts on whether d-mannose powder and marshmallow leaf/root tea are safe for IBS? Also, Natural Factors has replaced the glucose in their DGL tablets with stevia and xylitol. The primary sweetener is stevia and the xylitol is listed in “other ingredients.”
Hi
I have 3 questions I need help with:
1. There is no mention of FP and serving values etc for Lactose-free milk in the kindle edition I just downloaded on FTD for heartburn and LPR We normally only have lactose-free milk at home so it would be really good for me to know as I use it in my tea.
2. Regarding Jasmine rice, given its FP is zero, can I have as much of it as I want with every meal to increase my weight? However, I notice there is a serving size suggestion of 5.3 ounces/150g. A bit confused.
3. I had just Chicken Lettuce Wraps from Day 4 of the FTD diet plan. However, it says here that the dish serves 2. So, if I want to cook for one. Should I halving every ingredient?
Please can you clarify as I am so new to this diet.
Thanks
Seeme
i got a bit discouraged as a vegetarian reading your book; I had been trying to stay away from the processed soy (and dairy if possible) and had been depending on beans; for example, mung beans. Do you have any other suggestions for vegetarians to get our protein in? How about soy products such as soy protein powder?
What is the FP of sunflower seeds? Thank you.
Can this FTD be used with a child aged 10 who has symptoms of SIBO?
Within your calculation for FP I see no weight being given for fructans (onions and garlic). While on the SCD/SIBO diet I know that onions and garlic (unless infused in oil) were to be avoided. I tested positive for fructose malabsorption as well as SIBO so I am wondering if the onions and garlic should be avoided?
Please ignore my question, I see you addressed garlic and onions above and it wasn’t due to the fructans but the oligos. One gets the idea on the other diets that onion, garlic, peaches, watermelon, etc must be eliminated from ones diet while not really identifying when we should stop eating the foods that are legal during a given day,. Your approach makes much more sense in that we are staying within a given number of FP points per day. It greatly expands the possibilities of recipes we can enjoy while quantifying with points what we do eat so that we are eating a diet that will keep the daily FP down to a safe level…
After just one day on the diet all of my heartburn symptoms were cured. Incredible.
But what I don’t understand now is: what’s next? Is SIBO a life long problem for which I’ll always need to manipulate my diet? Or once my intestines heal can I go back to eating as I please?
I made the mistake of attempting 1/2 an English Muffin very soon after my symptoms were gone, and the heartburn came right back. Does this mean A. Even though my symptoms are gone, I still need more time to heal? B. No more gluten for me ever again? C. Do I need digestive enzymes? Or D. Will I need to continue this type of diet long term? I’d love your guidance on problem solving with my diet once the symptoms are gone.
(One last sidenote – I had chronic heartburn for about a month after I had to take two doses of antibiotics for bronchitis. Your book saved me!!)
Thank you,
Stephanie
Dr. Robillard,
Thanks so much for your books and especially for answering questions. I’ve read the Fast Tract Digestion IBS and the one for heartburn. I’ve been cooking and enjoying the recipes for some weeks now, and have had good improvement in my IBS – Diarrhea. However, I still need help with the GERD. I have hiatal hernia and I believe I have bacterial growth even in my stomach because I belch so much, even first thing in the morning when I haven’t eaten anything for 12 hours. Consequently, per your advice, I’m now avoiding all rice, potatoes, and wheat, and the only carbs I’m getting are from 3 servings per day of the low-FP fruits.
My question is this: how long should I continue on such an extremely low-carb diet in an attempt to starve bacteria in my stomach?
Thanks,
Joy
I just bought the book and was planning to start the Fast Tract Diet soon. I was wondering what I could substitute for the Almond Flour in a few of your dessert recipes in the Fast Tract Diet? I am severely allergic to tree nuts. I was wondering if I could make Graham cracker crust instead, since it says on the FP chart that graham crackers have a low FP. Also, do you have any suggestions for alternate snacks to substitute for the Snack mixes containing nuts? Thanks so much!
I am currently reading Fast Track Diet IBS/SIBO and love that you have menu planning in there. However, I have many food sensitivities right now including eggs, chia seeds, bananas,and most nuts (expect raw almonds). Also have been gluten free since 2006. Currently I am dealing with severe case of SIBO and would love some ideas on alternative protein sources aside from eggs & nuts for breakfast meals. I prefer to not have animal products with every meal.
Two more questions:
1.) Organic Natural Value coconut milk (guar gum free/BPA free). I can not find the GI to calculate the FP. I read a while ago that coconut products are hard to digest for IBS, etc people but wondering if you have found other research to dig deeper into that statement. Coconut oil work fine for me as well as the can full fat milk (small portions). Just not sure if I am hindering my healing process by using it.
Natural Value: Total Carbs 7g, Dietary Fiber 1g, Sugars 2g (Serving size 1/2 cup (100g)
2.) Mary’s Gone Crackers Super Seed Crackers. They do not list GI on the website. I read you mention brown rice & quinoa being on the moderate to high side of FP but in the small amount used in these crackers would it be safe to consume less than the serving size without hindering my healing process?
Total Carbs 19g, Dietary Fiber 3g, Sugars 0g (Serving size 13 crackers (30g)
*Organic – *Whole grain brown rice & *whole grain quinoa, *pumpkin seeds, *sunflower seeds, *brown flax seeds, *brown sesame seeds, *poppy seeds, filtered water, sea salt, *sea weed, *black pepper, *herbs
Crackers are baked.
Thank you!!!!
Melissa
After rice flour made from jasmine rice, how would other GF flours rank as far as their fermentation potential? Any idea about the FP of tapioca flour, potato starch, sprouted oat flour, sprouted corn flour?
Three months ago I had been on PPIs for two years and began suffering more severe reflux. My doctor told me to double my PPIs from 40mg per day to 80mg per day. Instead I read your book, started the diet and found immediate relief. However, I am still slowly weaning off antacids due to acid rebound. I am completely of Prilosec and I am now down to 30mg of famotidine(Pepcid) per day. I would like to try to stop all antacids in the next 4-6 weeks but would like to have a back up treatment for travel when food is less easy to control. What are your thoughts about DGL(deglycyrrhizinated licorice extract) taken before a meal as a heartburn preventative? These are chewable tablets with 1 gram of sweetener per serving consisting of fructose, mannitol, and sorbitol.
I have SIBO which I has been under control for since January this year with a very restricted diet and Biotics supplements specifically prescribed for the condition. About a month ago, however, I developed extreme indigestion, which my kinesiologist diagnosed as gastritis and acid reflux and advised me to stop taking all my supplements and begin taking 150 mg of ranitidine twice a day, which I got from my GP and which helped for a while, but now the condition is persisting and seems to arise unpredictably.
I discovered your site recently and apart from all the other carbohydrates I am not eating, also withdrew fructose in any form, and for an afternoon and evening I was symptom free and thought I had solved the problem, but yesterday the burning sensation in my chest returned for most of the day and evening.
I am awaiting your book and so I don’t have the full picture as yet and the only thing I can put this down to is either stress, or that I have not been measuring how much quinoa I consume and that I could be well over the 45 grams of fermentable carbs in doing so, or that the Trader Joe’s almond milk I use which has an FP of 3 for 8 oz, I just noticed contains gellan gum and zanthan gum, both of which are not allowed on the Sibo diet.
What would you suggest would be a good next step for me?
Dr. Robillard,
Thank you for the pre-calculations you’ve done in the 16 Tables of foods. However, I’d like your suggestion on how best to use them since the numbers are in ounces and grams and need to be converted to ordinary household measures in order to know how much food we’re dealing with (teaspoon, tablespoon, cup, etc.) I have been unable to find any conversion table on the internet that gives the amounts in volume that you present in weight. It requires buying a scale or visiting the grocery store and taking down all the label numbers for each product in which you’re interested…particularly if you want to compare brands. Any ideas, or am I missing something? I was very glad to see normal household measures in the recipes.
In Food Table #3 “Rice Cakes” is mentioned 3 times. Once for Low-amylose rice, once for high-amylose rice, and once for puffed rice cakes.
Although I am more interested in the rice cakes, it’s the same with rice itself. Besides jasmine which seems to be best, there’s short grain, mid grain, long grain, waxy.
Can you please tell me how to find out which kind of rice cake is which? Amylose is not an item that’s labeled. Would I have to call the company and see if their customer service people know what I’m talking about?
With rice, is long grain BY DEFINITION high-amylose, and so forth for the other types? Thank you in advance.
I am perplexed that the Fast Track Diet and the FODMAPS Diiet say the exact opposite from one another on resistant starch. I just don’t see how both approaches can be right.
My question today is about a recipe (not one of yours) that contained all “approved” foods but made me ultra-miserable the next day. It was a sauce for fish or chicken: 1 cup cherry tomatoes, 1/4 cup roasted red pepper, 1 clove garlic, minced, 2T extra-virgin olive oil, 1 T capers, 1/4 t kosher salt. DELICIOUS! I used 1/2 t of minced garlic from a jar instead of mincing my own. I used about 1 tablespoon of the sauce only. The garlic is the only ingredient I can think of that would have bothered me, but I used less than the recipe called for, and for my own portion, just a small bit – whatever was in that tablespoon of sauce. Any ideas on what happened? Could this mean fructans really do matter? Thanks if you have a chance to respond.
I am wondering if Stevia is okay on this diet? I am also wondering about an appropriate protein powder to put into smoothies. I have been on the FODMAP without much success but using a FODMAP approved rice protein powder, which sounds like I should change in doing this diet Thanks!
Hi Norm,
I would love some tips since I followed the fast track diet for over 3 months while taking Biocidin drops 3X a day & a Theralac probiotic but my second breath test came back worse for SIBO. Feeling so confused and frustrated. Both times in the severe range with 2nd time worse. What I’m I doing wrong?
Thank you for any guidance you can give.
Melissa
Hi Melissa,
Sorry to hear about your experience while on the FTD. It’s not possible to fully assess / address your situation in this format, but here are a few suggestions:
Review the trouble-shooting sections in the book and be sure you are limiting FP points in line with your symptoms. Some people need to go to 25 or less per day. Also the pro-digestion behaviors for choosing, preparing and consuming foods are critical. Once you do that, re-read the chapter on underlying conditions which may contribute to SIBO/dysbiosis. Other underlying conditions (beyond simply consuming too many fermentable carbs) if they exist must be identified and addressed. If all else fails, you might consider our consultation program which you can find on this site.
Thank you for your speedy response. Based on your response, I’ve have been reviewing Chapter 8 over and over to make sure I don’t miss anything. Based on my reading which states ….”System can be disturbed by factors such as…autoimmune conditions including the drugs to treat them..” I am concerned that by taking Methylfolate Plus by Biotics 2x a day and GTA by Biotics due to my blood work being low, that may have hurt me more in the end. Also, based on my IgE blood work there were many foods I was unable to eat even those considered safe in your book so it was super hard to find items to eat. I thought by eating Mary Gone Crackers Super Seed I was doing good but again I feel I may have made matters worse. Essentially, those crackers were my go to if I needed a small snack or used instead of bread (since I can’t eat eggs & eggs are in bread). While I know flax, whole grain brown rice and quinoa are on the higher sides of fermentable foods, I thought since its in cracker form the amount of each would be minimal. Especially since there are other seeds in there. Was I wrong to conclude that? I will be discussing tomorrow at my doc appt about all the underlying causes to see what we can test for further.
Thank you again for your previous quick response.
Melissa
I just purchased your book, you are the first person who seems to have both the science and the understanding. Thank you! My experience with a gastroenterologist was being told to see a hypnotherapist because I was (she insinuated) swallowing air. Love it!
Your book says that FLAX seeds are moderate – yet ‘no carbs’…..Not sure I understand. I LIKE them! .Like wise I suppose chia seeds are out of the question? I had thought that both these, seemingly going through virtually unchanged, would have given little sustenance to bacteria…
BTW I have always been so healthy, or so I Thought, exercising heaps meant I had to eat heaps, the more complex the carbohydrate the better… I made myself into a vat of bacteria!, I am so hoping this helps….
thank you so much, Veronica (Australia)
Hi Veronica, With Flax and Chia seeds, they are both mostly fiber and fiber is fermentable. Hopefully most of the fermentation will occur in the large intestine. But the Fast Tract Diet limits all fermentable carbs (at least until symptoms cease) to be on the safe side. But FP is all about serving size. 1 tablespoon of either seed type keeps the FP to 5 grams or less.
I am trying to better understand the prep of Sushi or Jasmine rice and Resistant Starch. I’ve read some of your articles posted here and of course your book, but while you say how to prepare the rice with washing and soaking, I missed anything on how to keep the resistant starch away once cooked. If the rice is prepared earlier in the day, but remains in the pot on the warmer, does it keep it from becoming resistant. At what point in the cooling process does it become resistant? How fast from pot to freezer must it go? And then when it comes out of the freezer, can I simply defrost in microwave before eating. Want to make sure I am not messing up my FP with the way I am preserving my rice once made. Thanks much!
I have lost more weight than desired on this diet and wonder if you have recommendations for high caloric foods with low FP. Is there a nutritional drink one could have to supplement that is low in FP? I am thin to begin with and have lost about 18 pounds since June (when I started diet) and really haven’t more to loose. I can’t seem to gain anything back. Appreciate any suggestions for weight maintenance. I find it very difficult to eat 2,000 calories or more on this diet without gorging on fatty meats. On the positive side, I have had a lot of relief from pain from about mid August to Mid December. I am having a setback these last two weeks. Probably because my FP grew higher than I thought as I added in a few more things in the effort to gain weight. Unfortunately, my symptoms don’t present right away. Once they start, it’s too late and it takes a few weeks to get it back under control (back to baseline and I fear more weight loss). Appreciate any help with allowable high caloric foods or ways to gain weight but staying within FP guidelines.
Hi Shawnie,
This question has been addressed in one of the Q&A Posts. One other solution is to get the new FTD Mobile app (https://bit.ly/1QPtAmu), which lists over 800 foods – more low FP choices.
As I understand it, the fast track diet aims at starving the bacteria. However, can it truly eradicate them from the small intestine? If the food restriction is continued for a long period of time in an effort to kill the bacteria, aren’t we also starving the bacteria in the large intestine? Can the diet alone clear the bacteria once for all, as this is what SIBO sufferers are aiming at? Thank you.
Hi Micol, This is a good question, but it has been addressed here (Scroll or search for “IBS and Gut Microbiota Question: The Fast Tract Diet seems to starve all types (good & bad) of gut bacteria for my IBS”) and in other places on this site.
Thanks much, Norm. I have a couple of follow-up questions not specifically related to the diet but to SIBO, I don’t know if you can help answer them:
1/ what is the relationship between SIBO and anxiety. Often doctors think that it is anxiety to trigger our digestive disorders, but in the case of SIBO/IBS it seems the other way around. How does SIBO affects the nervous system?
2/ Is it problematic to become pregnant for a ‘chronic’ SIBO sufferer? I am specifically referring to symptoms that can exacerbate during the pregnancy and possible consequences for the baby’s health?
I am trying to figure out my health problems. I have lots of food allergies, eczema and urticaria being my initial symptoms. However I restricted my diet to a low histamine one and although my symptoms improved I now have chronic constipation even though my stools are soft. I am wondering if I am eating too much fibre for whatever is going on in my digestive system. I am also very bloated by the end of the day
Hi there, firstly thank you Dr Norm for your really helpful book. I’m just beginning on the FTD (it’s my first week) and I’m still suffering with very bad reflux and LPR. In order to get some sleep, I’m forced to take a reflux suppressant called Rapidol. It contains sorbitol, a sugar alcohol, which I know from your book can cause fermentation. I can tell it gives me bloating and pain but without it, I completely lose my voice and have intolerable pain in my oesophagus and throat. I can’t limit the medication until the reflux eases but the medication itself could be causing more reflux, so I’m not sure how to proceed?
Hi I like yourself have intolerable pain in my oesophageus and throat and have had good results on the diet for two weeks but now am experiencing symptoms have tried cutting back and following everything religiously , have lost so much weight too…what is the pain I am experiencing ? Hope you have had some joy in your symptoms !
Your work has been very helpful and I’ve found that by very strictly limiting vegetable matter I can largely control the “fire in my belly”. However, I continue to have chronic diarrhea (once a day on waking). Any thoughts or suggestions?
I have your book and am planning to try the diet. However, you suggest for best results to follow your menu plan for the first 2 weeks. But I don’t see how it would be possible for someone (like me) who works full-time and thus can’t cook those meals listed.
I got you Krambo. As long as you keep your daily FP points low (choosing low FP foods) you will be fine.
Hello,
I have been on a vegan diet for the past 5 years. I have been having symptoms of acid reflux, the doctors think it may be related to a hiatal hernia but they have not confirmed. How can I follow this diet as a vegan and vegetarian? i read the book but I struggle to apply because a lot of it is meat based. Thank you!
Hi Jen,
I can appreciate your situation. Since some go-to vegetarian foods such as legumes and whole grains have high FP values and need to be limited. This presents some challenges. Here are a couple of resources that might help. You can discuss this issue on the Fast Tract Diet Official Facebook page. You might also read this review on Amazon for Fast Tract Digestion Heartburn: “I got my voice (and life) back, this really works – (from a low-fat vegan viewpoint) By Chas in Los Angeles on February 28, 2015”
I have a chronic cough which I believe is related to silent reflux. The PPI the doctor gave me didn’t work. I am adhering to the Fast Tract Diet rigorously but also avoiding caffeine, acidic foods, etc. I use some fats in cooking but not a heavy amount. I am taking TUMS with my meals at present because it seems anything I ingest, even water with medication, results in another coughing fit. Hopefully the diet will fix my coughing and I can eliminate the TUMS. I applaud you for your excellent research helping so many people. I hope it can help me.
Thanks Nancy. Give it some time and you need not fear fats.
Hi Norm,
the fast tract diet app tells me that aged cheese is okay/has a low FP. I’m just wondering if there is a difference between raw and normal dairy? I usually eat aged raw milk cheese. Also does it make a difference whether it’s cow’s or goat’s milk products? I just wanna make sure I’m doing it right. Thank you so much in advance!
Can a person that has gastritis use the Fast Tract Diet just as it is? Or are there more things a person may have to be careful of, such as alcohol or nicotine, or other foods? The person I know that has gastritis also has gerd, and also tested positive to SIBO.
What is the FP of mustard?
Hi Ira, Its zero.
Hi Norm! Just ordered your book and can’t wait to get it and get my GERD/LPR resolved. I’ve been reading everything I can until it arrives. My question is this, I’ve had my gall bladder removed. Should I take a supplement to aid digestion?
Thanks
Hi there. I was recently diagnosed with LPR silent reflux. I’ve been suffering for this for many years, however, was just recently diagnosed with it. The past few years my breath has progressively gotten worse. It’s so bad to the point where people can’t talk to me even from across a room. Obviously, this has ruined my social life, romantic life, professional life and pretty much relationships with every single person I encounter. I’ve become a recluse. It’s worsened my depression and anxiety. Will this symptom go away if I can cure my silent reflux. I’m scared nothing will work. Im a 35 year old beautiful smart woman who has so much to offer the world… I want to be able to be myself and live life to the fullest. I used to be happy. I want to be happy again and I want to be able to talk to people again. I shouldn’t have to life alone scared and helpless. Thank you for your research and for writing this book. The 2 week induction diet that you have in your book, should that be followed as it is exactly listed and after the 2 weeks refer to your food list? Do you think my breath will be normal again – clean and fresh. Do you think your diet modification will work for my reflux? Please help. I’m scared.
What kind of toothpaste and mouthwash do you recommend? You had mentioned that most have sugar alcohol in ingredients. (?)
Hello, thanks for your insightful book! I have been following the diet for a few days (the app is a huge help, by the way!) and I was wondering if blending greens/fruits in a high performance blender such as a vitamix reduces their FP. I usually have a green smoothie for breakfast, which sets me back 10-15 FP even if I seriously reduce the fruit to the bare minimum. I could see how the mush that comes out from a vitamix is easier to digest and thus has lower FP… Thanks!
Interesting question Michael. Most juicers remove some of the insoluble fiber which would be expected to reduce the FP. Since I don’t know exactly how much of a reduction this is, we recommend people add up the FP values for all veggies and fruits used as the most conservative approach.
I have had GERD for 3 years and last year I was diagnosed with Fructose Malasbsorption. In last year I followed the Low FODMAP diet, but it does not relieve my symptom. A few days ago, I read your book, Fast Tract Digestion- Heartburn and determined to follow your guideline. One question I have is about apple cider vinegar (ACV). I have taken apple cider vinegar (ACV) 30 minutes before every meal to facilitate acid production in my stomach, but I found that some insist that ACV should not be taken for fructose malabsorption because of fructose in it. However, in the Fast Tract Diet app, ACV has 0 FP. I’m very confused. Would you recommend drinking ACV? Thanks.
Hi, I just read your book and was wondering whether your recommendations on herbal treatments (“antibiotics”), not mentioned in your book, are the same as for pharmaceutical antibiotics. I prefer to use either as a last resort if diet for symptom control is thorough enough for long-term health of the digestive system. Thank you.
Good point J. Yes, I do view all antibiotics under the same umbrella. Of course, there are many differences. Some kill, others inhibit. Some are produced by bacteria, some by fungi, some from plants/herbs and some are synthetic. But each has a particular spectrum (range of which types of microbes they are active against) and strain-specific potency. At the highest level, I think diet first and antibiotics only if all else fails. Even then, you need a careful approach to avoid numerous potential pitfalls linked to antibiotics.
I read the book, implemented the dietary adjustments, got immediate relief from heartburn…. Yipee!!
My friend who was recently started on a diabetes med wonders “How does this food plan interface with a diet recommended for controlling blood sugar”
Thanks, I’m telling anyone who will listen about the plan!!
Hi Karen, The diet is flexible. People with diabetes need to watch their blood sugar levels. Carbs need to be limited including some of the low FP but higher carb, higher GI carbs. To help in this regard, the FTD limits carb counts in the recipes to approximately 75 grams/day. This is lower than most standard diabetes diets, but it may be wise to lower total carb counts even more to be sure blood sugar levels are fully contolled allowing people to depend less on medications.
Ty
If I can only afford one or the other, would it be better to purchase the downloadable book or the app for iPad?
Hi Francine, The app will help you jump start the diet. Read the Fast Tract Diet chapters in the app before starting the diet. This is important. I would also recommend reading the book, so that you can fully address your issue(s). Good luck.
Is it ok to eat apple?
Hi Norm,
i have your book for IBS and iphone app. coudn’t able to figure out how to calculate FP for “Unsweetened Vanilla elemental drink”
can you let me know the FP for Absorb Plus “Unsweetened Vanilla elemental drink”.
you can find the supplemtanl facts information of abosrbplus in it here.
https://shoppe.listentoyourgut.com/absorb-plus-unsweetened-vanilla-1-kg-tub/
Hi Norm, I have recently started on the diet after suffering from daily reflux for about 18 months. Early indications are positive but I was wanting your thoughts on the supplement slippery elm powder I.e. Whether this is counter-productive to the diet. I’m struggling to find much information on it. A dose is 0.5g carb and 3.4g fiber. Thanks Richard
I am a Type ! diabetic and am concerned about the easily digested starches in the Fast Tract Diet. Do you recommend just leaving them out or using another diet? I have heard you recommend the ketogenic diet for diabetes but I have not found that on the website or in the book yet.Thank you!
Hi Melinda, Great question. Low FP foods are either small servings, low carb or high GI. While most of the low FP foods in the tables are lower carb (the vegetable table is a good example), some (especially starches) are high GI and high carb. Limiting these is a good idea for diabetes or other metabolic sensitivities. The recipes in the books total approximately 75 grams per day which is certainly lower than the typical American diet, but I agree, you may need to reduce your daily carb grams even more. The ketogenic diet is a great alternative my view.
Thank you!!!
Hi Dr Robillard,
I recently bought your book and really like the concept! I am working on putting it into action.
Is the diet okay for someone with hypoglycemia? I am concerned about some of the high GI carbs that have low FP. However if I just do low carb in general, I will will lose weight and I don’t tolerate fats well to replace with those. I am already on the thin side as it is and reducing carbs too far will cause a problem.
I have been combining fats and carbs to slow blood sugar release but does this cause the carbs to be more fermentable? for example, i eat rice crackers with sunflower butter.
How do you calculate FP when there are multiple foods together such as in a gluten free flour or cracker?
I couldn’t find these answers in the book and need them to be able to be successful with the diet. thanks for all your work and responses! Sincerely, Molly
Hi Molly, I hear you about this concern. To avoid SIBO and a wide variety of symptoms and conditions involving imbalances in gut bacteria it’s important for many people to moderate the amount of hard-to-digest fermentable carbohydrates we consume. At the same time we want to keep blood sugar from extreme fluctuations. A very low carb diet is one way to do this since your liver will produce the required amount of glucose from gluconeogenisis. Another way to accomplish this is to introduce some carbs but focus on low GI carbs. The problem with the low GI carbs is that they can overfeed gut bacteria. The FTD is aimed at controlling fermentable carbs, but allows you to do it with a low carb approach or by adding higher GI carbs. Implementing the higher GI carbs approach in your case, may take some finessing. Smaller but more frequent meals may be one way to do this. Another thing that may help is getting a glucose meter if you don’t already have one so you can monitor your blood sugar real time helping you make finer adjustments.
I am wondering why pumpkin seeds are considered to have a high FP because if you use the FP calculator they come out as having a low FP. Am I using the calculator incorrectly?
Hi Kristen, I did the calculation using a one ounce serving containing 15 grams total carbs, of which 5 grams are fiber. I entered a glycemic index value of 24 (based on similar foods which have been tested) and got 12.6 grams FP which is rounded to 13 grams. Please check the values you are entering and give it another try. You should get the same answer.
The label on my seeds (superseedz brand) says total carbs are 3 grams and 2 grams of dietary fiber. That explains the discrepancy. A general search for pumpkin seed nutrition on the Internet shows what you are reporting, 15g of carbs and 5g of fiber. Any idea why there such a difference? I cannot eat tree nuts or sesame due to allergy so I was sorry to see the FP of pumpkin seeds was so high.
That would explain it. Kristin. Is the 3 grams total carbs / 2 grams fiber for the same serving size of 20 grams? I will keep my eyes open on this. If the serving sizes are the same, likely one of these values is incorrect.
Serving size is 28g/1oz
got it.
Hello… I have extreme GERD & take Prevacid. In fact I have taken it daily for 10 plus years and now have Osteoporosis.
I have read your ebook and downloaded the APP. I cannot find advise on what a daily target would be for FP Points.
Please advise.
Many Thanks, Colleen
I experience noticeable gas and bloating even after eating proteins, such as fish and eggs (zero FP), on their own. I understand that some bacteria can ferment amino acids and assume this must be what is happening. This makes me concerned that the Fast Tract diet won’t work for me, as although my daily FP intake is low I’m still experiencing symptoms after zero FP meals, which makes me think the bacteria are not being deprived of their food source and therefore may not decrease in number. Do you have any thoughts? Many thanks.
I developed LPR 5 months ago and just started the FTD last week. I realized that by day 4 I cannot tolerate dairy (it brings that phlegmy feeling back into my throat) even when using enzymes and I want to avoid dairy until my symptoms go away. The nut mix also tends to upset my stomach. However, I am concerned that my carb intake will be too low. I work out 6x a week and while playing tennis yesterday I felt very light headed and had to sit out. Am I getting enough carbs? Thank you.
Can you please respond to the review of the research by Dr. Michael Gregor, MD regarding plant based food diet for reflux. His web site is nutritionfacts.org. On the web site he has a video “Diet and GERD Acid Reflux Heartburn”, Volume 24 May 22, 2015 which says, among other things, that fat is the culprit since research shows it relaxes the LES. I was ready to adopt Dr. Robillard’s diet strategy, but now feel the research is less supportive of his thesis. I have been on PPI’s for 15 years and have had made several attempts to go off them. I am currently still taking them and they don’t seem to be working as well as previously.
My main goal is to find the right strategy to help me resolve this difficult issue. I am not convinced including animal fat and eggs in my diet would be helpful. I would appreciate your response to Dr Gregor’s research review which leads one to believe a plant based diet would be more appropriate.
Hey Cindy
What approach did you try and have you had any success/advice?.
Hi,
This diet really helped me. After three years of searching for an answer it only took a day for my symptoms to improve on the Fast Tract Diet. I just have a quick question regarding the app vs the book. Why would 80g of parsnips in the app be 9FP but only 3 according to the book? If in doubt should there be more like this should I follow the book or the app?
Thanks
I had a question about the FP for Warrior Food’s Natural Vegan Protein Supplement in your APP. It shows the FP at 1g, but the ingredients in this supplement is sprouted brown rice protein and pea protein.
Is the FP reduced because the brown rice is sprouted and also a concentrated protein?
Thank you.
Yes, it’s the latter Parrizia. Because this is a protein isolate, there are few carbs. Protein is not assigned any FP points.
Does parboiling rice affect the amylose in it? There is a variety of white basmati rice that is parboiled and is called “yellow rice.” The grains do not stick together so I believe that there is much less starch in it.
Thank you.
Probably not Patrizia. Though I don’t see an entry for “yellow rice”, there are several parboiled rice varieties in the glycemic index database. With the exception of parboiled Sungold, Pelde, white low-amylose rice with a GI of 87 (giving it a low FP), the others had relatively low GI values (high FP).
Herbal Teas like Camomile were not listed on the Food List in the Fast Tract Digestion Heartburn Book. Yes/No?
The mobile app includes Teas – Zero FP points.
Thank you Norman. I will get the app.
Norm,
with such a high protein, low carb diet, how do you address motility issues? I am going from a mostly vegan, high fibre plant-based diet to following the FTD due to SIBO and am finding that motility is affected and also I am wondering about high glycemic foods such as jasmine rice and potatoes contributing to inflammation. Also, my pH has dropped. Thank you.
Norman, is there something you would recommend during the first few weeks of strict adherence to FTD for sinus congestion/excess mucus? My lpr manifests in sinus symptoms and most remedies are not FTD friendly or may lower stomach acid. Thank you.
I bought the book. Love it. But a FP of 1 for a white baguette? Is that possibly a misprint or is that, for me, a dream come true?
Thanks. Collin
Funny. No misprint. But do use caution, eat slowly, limit serving size and chew well to optimize digestion.
Hi,
I started having GERD syptoms about 6 wee ago.
I was doing a ketogenic low carb / high fa diet when the GERD started, which initially made me think that it was the low carb / high fat diet that caused my problem.
Since I was already on a low carb diet, does it make sense for me to try it again?
In addition to the low carb diet I was drinking a lot of coffee when the GERD began.
Any help is appreciated.
Sincerely,
John Connell
Norm, raw honey is known for containing digestive enzymes including amalyse. Any advantage? Does it get any FP grams credit? ( fingers crossed lol!)
Interesting idea Robert. I’m not sure honey amylase will do much after passing through the stomach given the low pH (The optimum pH for honey amylase is pH 5.3–5.6, but I’m not sure about it’s stability at very acidic pH). I personally use small amounts of raw honey – in the teaspoon range. The FP value is relatively low. I agree with you that raw is best. It would be great if it helps digest starch, but I wouldn’t depend on it.
Thanks
Norm. Really enjoyed your book. Just started FTD about a week ago. Good results so far. Thanks for taking the time to answer questions on this forum.
Have yet to read the book, that will be my next step. However I happened to see Prescript Assist on your store page, which I just looked in to this week. I found this article, basically the crux of it being limited data re: safety, etc of many of the soil-based microorganisms: https://fixyourgut.com/hso-probiotics-part-3-prescript-assist/. Can you comment? Thanks in advance.
Thank you for your great book. I have been on a PPI for many years and wish to get off them. I have started your diet but it is very difficult because I am Vegan. I have decided to include the yogurt and butter for the three weeks but I find that I have a greatly increased anount of stomach gurgling. Is this normal? Also I would like to eat lentils and beans eventually. I researched the vegan /vegetarian version of Beano which is BeanEze and found that it contains Sorbitol and Mannitol. I suspect that Beano may also? Is it still safe to take this? Thanks for your help.
Hi Norm,
I’ve been on the fast tract diet for around two months now and have been keeping to it very strictly. I’ve been weighing all my food and making sure i don’t go over 35 points a day but usually keeping to 30. I’ve also been staying away from things that can irritate the gut such as coffee, alcohol and gluten. Immediately from day one I felt a huge improvement. (Thank you so much for this diet and app) Over the last three weeks however the symptoms have started to come back and have been getting worse. This started the day after I started going to the gym again. Is there any relationship between heavy exercise and SIBO or is it possible that I’ve just become immune to the benefits of reducing FP points. There has been no major change in my diet from week one when I was improving to now when i’m getting worse again.
Thanks
Hey Stefano, Changing your diet involves many variables including macro and micronutrient changes, adjustments by your body and metabolism as well as changes in your gut microbe populations in response to diet changes. In theory gym work outs should drive calorie demand which is a good thing, but it’s hard to pin point what’s going on with out lots more info including food logs
One thing you might try is diligently limiting FP points even further short term and perhaps experimenting with avoiding certain carb types such as starch, for instance. Feel free to contact us under the consultation page for more hands on support.
This diet has been a godsend. My 6 yr old daughter has celiac disease and possibly lactose intolerance; but, a gluten free, dairy free diet wasn’t helping. Nor was the specific carbohydrate diet. She was daily rolling on the floor, shaking in abdominal pain, couldn’t even walk sometimes and we couldn’t figure out why. We started to get a clue when we noticed she had really bad breath (correlated with fructose malabsorption). With this diet, the pain was gone almost immediately and has been gone for a month (since we started the diet). We’re so grateful! Thank you!!!
We’re guessing that celiac disease damaged the villi which also caused fructose malabsorption, lactose intolerance and led to SIBO (or something like that). We’re just trying to figure out a few things:
1) Due to size and weight, does a 37 lb, 6 yr old child need to have a lower daily FP total to adhere to than an adult? We had been keeping it pretty low – maybe in the 20s. Should we just slowly introduce higher FP foods and see how she does?
2) How long will she need to adhere to the fast tract diet? Until the villi have healed/grown back on the gluten free diet? No idea how long that is (never had an endoscopy – still on the wait list to see a doctor).
3) Lastly, we noticed that many of the FPs in the book, do not correlate with the FPs on the app. I thought the app would be the most updated version so I was going with the FPs in the app; but in a previous post, you say to instead just go with the most conservative one?
Thanks again for your help!
Hi Norm, Just caught sight of Stefano’s story. The gym is the problem. Vigorous exercise is not good for GERD sufferrers. Something I discovered the hard way. Being a dancer I have since discovered that if I dont jump around and bend over(yoga/ pilate type stretches) then it is okay. I’ve been advised to exercise at least 4 hours after eating as well and try to stay upright when stretching(no lying down) and keep impact at a minimun. No jogging, walking is fine. Swimming and cycling up right is fine etc.
Now back to me: I’m not good with dairy, and I don’t eat lots of eggs etc, so the recipes are going to be hard to adhere to. I would love to try the 30FP per day concept however. Looking at Table C(I don’t have a smart phone for apps) it states the GI reading and not the FP. I cant get my head around the maths, sorry! Could you just simply tell me what 50 GI translates to in FP and I can use that as a measure. I must admit I was hoping that Table C food groups were defined in FP and not GI. Finally, I take it, basically, that GERD sufferers are better with food that is low GI. Which is contrary to all the advice out there that keeps advocating high GI food for health.. thanks for your time.
I agree about the vigorous exercise Nella. The tables in the appendix of the books do list the FP values. You may need to adjust your device a bit to see them. The tables are designed to be responsive to a wide variety of devices so you should be able to do this.
thanks for that, how stupid of me. I had the contents up at the same time. I appreciate your prompt response!
No problem Nella. Could happen to anyone.
Would you be able to recommend what might be an appropriate maximum daily FP for someone who probably has SIBO and definitely has blastocystis along with overgrowth of streptococcus in the large intestine? I assume from what you say in answer to other questions that normally in these circumstances it would be good to cut out or minimize starches, but does this still apply when someone is very thin and seems to do much better on a little jasmine rice than on squash, for example? Thank you for your book and your efforts to unravel these mysteries.
Hi Norm, can you advise me on carob? I like to make my own carob chocolate. two of the main ingredients are carob powder and raw cocoa butter, all the other ingredients you already have listed in the book. thanks
Respected Dr. Norm..
I have severe belching, burping , heartburn feeling since last 7-8 months,,,,,,,,,,,,,,Used a lot of medicines like antacids,, PPI’s ( nexium 40mg,,, Risek 40mg, Omega 40 mg) etc……but doesn’t cure……….Only when i use medicines, heartburn sensation reduces but burping and belching still over there,,,,,,,,,Now i have also throat problem,,,,,,,,Can you please help me in this regard???????????
It seems like there are basically two perspectives on LPR. My understanding of your perspective is that it is SIBO. Not everyone who has LPR has SIBO. The other main perspective is Dr. Koufman and her outlook is about excessive pepsin in the tissue. But many people who have LPR have low stomach acid not high stomach acid. Not every one has drank soft drinks or eaten the type of diet she describes as a causative diet. All very confusing.
How can I transition from a low-fat, high carb “dropping acid” diet to the fast track? I have LPR-I weened myself of PPI’s, but when starting the new, higher fat and acidic foods allowed on fast track, experienced throat burning, airway discomfort and coughing. Originally, Medication did not eliminate symptoms, and low acid helped about 60%. Since I have been bothered by heartburn and gas(flatulance) I was hoping your diet was the answer.
Hi Anne, Since low acid, high carb did not provide a complete solution, I recommend giving the FTD diet at least two months since LPR symptoms are slow to respond to diet changes compared to simple heartburn for instance. I would also adopt the most stringent form of the FTD for at least two months keeping your FP levels below 25 points per day. Check out the troubleshooting sections in the book and FTD mobile app. Good luck. Other resources that may help include the Fast Tract Diet Official Facebook Group and on this site, the FTD Q&A page and our consultation program.
Dear Dr. Norm,
Thank you soo much for your work, the book and the application!
I’ve just started using it and reading the IBS book.
I have a question in connection with the app.
I’ve started to write my foods in daily basis in the app and my symptoms too.
Can I export them somehow to pdf or e-mail? I’d like to print them and give to my nutritionist.
Thanks a lot!
Hi Helga, Thanks for trying the diet and the mobile app. Currently the app does not have that capability, but I see how it would be useful. We will consider something along these lines in the future.
I also suffer from constipation. I used to drink 8 glasses of water a day. Now when I try to drink more water, my reflux acts up. How can I up my water intake to help control the constipation?
Hi Alana, Perhaps 6 glasses of liquid including other drinks as well would be enough. Further restricting carbs will also help.
Does the fast tract diet help reduce or eliminate symptoms caused by ulcerative colitis. I have read through a ton of material, but have yet to see ulcerative colitis discussed or even mentioned
15 years+ on PPI’s will I ever be able to come off them?
I’ve been taking PPI’s for heartburn for years, I have general IBS, bouts of severe indigestion pain, constant belching and bloating and have also developed bouts of constant burning in throat and stomach which is nothing like my ordinary heartburn, not made worse by lying down and not relieved by PPI’s. I’m desperate to rid my self of constant pain and come off the PPI’s and wonder if this diet can help, I’ve read if you try to come off PPI’s you get ‘rebound’ reflux worse than before which doesn’t settle and you end up having to go an even higher dose of PPI’s to try and cure it. I am my wits ends and don’t know what to do, If this diet helped is there any hope of coming off this god awful medication after being on it so long?
I suffer from both IBS and GERD (LPR). I want to start your Fast Tract program, but I am not sure which book to purchase and follow…The book for IBS or the one for GERD? Please advise.
Hi Amy, Both books feature the Fast Tract Diet. But each has chapters on each condition. I recommend the Heartburn book. You can read lots about IBS on this website that will supplement the book. You might also consider the Fast Tract Diet mobile app to implement the diet.
Thank you for your quick reply! I will get the heartburn book and the app. I look forward to implementing this program and getting much needed relief! Kind regards, Amy
Norm,
I read that potatoes and soybeans have an enzyme that inhibits protease enzymes from breaking down proteins during digestion. I’m not much of soy eater but potatoes are a staple in my diet primarily red and Russet. Any issue with FTD effectiveness with consistent consumption of potatoes even FTD friendly ones?
Hi Rob, Yes, soy, potatoes and many other plants, especially grains contain protease inhibitors. Cooking destroys them for the most part. Hopefully, cooking will minimize any problems with these.
Hi Norm. 3 Questions…one, I read in the Gut Health Protocol that if we take probiotics with only a few strains, we create dysbiosis. Can you recommend which probiotics to take (and which strains they should contain?) I’ve read mixed reviews about SBO brands such as Prescript Assist. The one I’m taking now only has lactobacillus acidophilus and bifobacterium lactis in it. Is that ok?
Second,that book also says that it’s essential to eat soluble fiber and even resistant starch to avoid damaging the microbiome. Is it possible to eat soluble fiber and resistant starch while still staying low FP on the FTD?
Third, for weight gain, as long as it fits into a low FP daily calculation, is it ok to eat sweet potatoes and white potatoes?
Thanks for this board and your work!
Do freshly made green juices (kale, cabbage, cucumber, chard, collards, etc) have high FPs?
Hi Beth, When using a juicer, some of the insoluble fiber will be removed so the FP will be a bit less than the ingredients. But the best rule of thumb is to calculate the juice FP by adding up the FPs for all the ingredients. My personal experience is that that juiced veggies are a bit more active in my digestive tract often leading to soft stools. This can be a good thing for someone who is constipated. But for me, an ounce or two of juiced veggies is plenty.
I have LPR that doesn’t respond to antacids (in fact, it seems worse on meds). My endoscopy was normal, other than the biopsy revealed “active inflammation of the stomach lining due to h. pylori.” I was treated with antibiotics, which seemed to help my symptoms a little, but it was short-lived. However, I read online that h. pylori doesn’t cause reflux. I’m at a loss as to what to do next. I have just started trying the Fast Tract Diet, even though I haven’t been diagnosed with SIBO. Is there anything else I should be doing or trying post h. pylori treatment? Thank you so much for any advice you may have. I’m feeling hopeless at the moment as LPR is taking away so much of my quality of life.
Dear Dr Robillard,
I have recurrent ibs/d and silent reflux so I’m trying to get it under control by doing your diet. I have tried low carb before and I got diarrhea and I’m worried this will happen again as I can see in week 1 there are hardly any carbs (apart from jasmine rice). Is there a way I can ease in or do I just have to go for it and hope I don’t react. I’m not sure if my issue is fat malabsorption or maybe my guts just don’t like change! Any advice would be greatly appreciated. I’m also worried I won’t be able to stick to the diet as I love my carbs. No more cakes, biscuits or cereal bars?
I. Read about “die off” symptoms in the SCD. They sounded quite intense. I tried that diet for 5 days but it didn’t seem right for me and my symptoms of GERD – elching, stomach pain, reflux, chest pain, never let up. I am just in day one of your diet and ate very low fp today and am still having quite significant symptoms. Is this die off? When might I expect some easing?
Several Clinical studies show that GERD can be caused by low stomach acid (hypochlorhydria), or high stomach acid (hyperchlorhydria). Both conditions will cause reflux, gas, belching, bloating nausea, abdominal pain, diarrhea and/or constipation, etc.. Diagnosing GERD without a pH diagnostic test, pH capsule test, or pH gastrogram is hit and miss. In most cases the miss, will result in a patient that has Hypochlorhydria (low stomach acid) being placed on a PPI. The end result of the this misdiagnosis is the patient may develop Achlorhydria (no stomach acid). Of the several hundred cases reviewed, over 60% of the patients with Hypochlorhydria were misdiagnosed and prescribed a PPI. Hypochlorhydria will cause malabsorption of the necessary vitamins, minerals and micronutrients necessary to keep the body healthy. It will also allow bacterial and pathogens to flourish in the digestive process. A pH diagnostic test, pH capsule test, or pH gastrogram is absolutely necessary for diagnosing GERD and other digestive disorders.
Hi Jacob, Can you please post a link to the studies showing GERD is causes by low stomach acid? In this blog, I found one case study where someone with achlorhydria suffered non-acid reflux symptoms and a study on people taking PPIs where 37% with reflux symptoms suffered with non-acid reflux. But for people not taking PPIs, the other studies I looked at were consistent with normal amounts of stomach acid in people with GERD. https://digestivehealthinstitute.org/2014/07/10/h-pylori-low-stomach-acid-gerd/
Hello Norm, There is so much information about probiotics, do you have any thoughts on how to use a probiotic in the best possible way? Also, I seem to remember you selling the Dr Ohhira probiotic and now you only sell the prescript assist. Do you have any thoughts on both these probiotics? Best regards, Albert
Hello Norm, is it safe to use a PPI over the short term to determine if I actually have LPR, or if it could be something else – chronic sinus infection. Also, if it is relax (LPR) and I am only able to partially control the LPR and IBS with the Fast Track Diet… is it necessary to go on medication (even just for a short term). My doctor keeps telling me that it would be worse to have acid in my esophagus/pharynx etc… as it can have cancerous implication in my future.
Hi Amy, This is a great question. I decided to dedicate a blog article to your question. You can find it here.
Can you tell us the FP Value of
– coconut aminos ?
And
– carob ?
Thank you!
Hello, thanks for all the great info and your book was very helpful.
I saw your comments about juice, that adding the FP value of each veggie should do the trick, however carrot juice is listed in your FP table in the book as very high FP, even though carrots have a low FP risk..so I am thinking that I am not understanding how to calculate the FP for juices..?
Thanks,
Pete.
What can be done to eliminate an overgrowth of Archea? They have entirely replaced a set of “normal” microbes in my lower GI tract. I have been on a low-fermentable as well as low-fodmaps diet and am desperately seeking an answer.
Hi Dr. Norm. I just ordered a copy of Fast Track Digestion – Heartburn. I’ve been dealing with Esophagitis for many years (it hasn’t become Barrett’s yet, so my Gastro tells me I just need to make sure things to advance). Previous gastros I’ve had have told me to take PPIs and H2s daily and just go on living my life “normally”. A new gastro had me take a breath test and found out I have SIBO – Hydrogen based. She thinks that resolving the SIBO might also improve my reflux/esophagitis. With the guidance of a seasoned nutritionist I just finished a 2+ month treatment plan of herbs + diet (gluten and dairy free + low FODMAP) and took another breath test – the result was actually a bit worse than before the treatment! My question is – does the diet that I’ll find in the book (Fast Track – Heartburn) address the different types of SIBO (Hydrogen vs Methane)? The nutritionist I’ve been seeing mentioned the approach should be different, so I’m curious. Thanks in advance and looking forward to reading the book!
Hi Dr. Norm. I was diagnosed with polymyalgia rheumatica-Autoimmune Illness for the last year. Given prednisone for the chronic pain. Saw a Functional MD. Diagnosed with SIBO. Have been on a restricted Paleo diet for a year and given 3 different herbal microbial protocols for the SIBO over this last year and treatments for parasites. 3rd test still came out positive for SIBO. Now they are prescribing the antibiotic Rifaximin. I’m worn out and still on steroids. Cant get below 15 mg per day without chronic pain. Any advice????
Today at 9:01 AM
Hello, Norm.
I’ve read your material and appreciate it very much. I have the app for the food potential list and am working on eating foods low in FP. I have LPR and throat is all phlegm constantly, trying to clear it, with no avail and affecting my voice, hoarseness.
I don’t think I saw anything about the cause of LPR where the sphincter at top of the esophagus is damaged, open, and am wondering if your diet addresses this, and if the diet, even with the damaged valve can help alleviate the symptoms like globus, of LPR in time?
I also notice that you allow 2 cups of tea, I just can’t seem to give up the green tea in the morning (1-1/2 cups); have given up coffee and a multitude of other things. Am a vegetarian so hard to find foods, but am going to adjust to it.
I thought I would give a try asking you about the sphincter damaged, and even with this damage, can your diet still help get rid of the phleghm (globus) constantly in my throat. That’s really the only symptom that I have.
I have had confirmation that a higher level of pepsin is in my throat areaas (Peptest) so am working on it.
THANK YOU
Have a good Xmas/Hannukah holiday.
Eileen Ruffer
eruffer@sbcglobal.net
Hello Norm,
I have a question about Jasmine rice. I guess that the Jasmine rice in the app is white Jasmine rice, because it’s 0 FP. Do you know what the FP of brown Jasmine rice is? Is it also low?
Thank you. Happy holidays.
Anna
Hi Anna, I don’t know the answer. I’m not aware of a published glycemic index for brown jasmine rice. YOu could try it or just play it safe with white jasmine rice.
I’m struggling with what I should be eating to get enough nutrients and energy for heavy exercise 4x a week. This is circuit training and weight lifting using many cross fit type elements. I’ve decreased carbs because of the FPs but I also have trouble digesting high amounts of fats. I had too much fat (healthy fat) the night prior and day of exercising, and I ended up getting sick because the fat hadn’t digested properly before I worked out. I saw earlier someone asked about this diet and exercise and you’d suggested that increasing fats with lower carbs would work eventually, but I don’t think that will work for me. I feel like I’m in a bad position either way. I wanted t increase my rice intake (jasmine & sticky) but isn’t rice known to constipate? Any suggestions?
Dear Norm
I have just dI have downloaded and looked through the Fast Tract App but I have a question I couldn’t find the answers to on the App.
If I have moderate SIBO symptoms am correct in assuming that I can consume up to 10 FP per meal if my meals are spread out every 3-4hours or should I be consuming 10 FP in total for the day ?
Hi Michael, There is a write up that explains the FP limits for the severity of symptoms. I itunes, you click on the more button, bottom right. Then click on Fast Tract Diet, then click “more” and you will see all the chapters. In android, you start by clicking on the “question mark” on the left.
Thank you so much for your reply.
Dear Norm
I noticed that you have measured the FP for the Absorb Plus Unsweetened elemental shake. Initially you said it was a 3 FP but that was before you realised it contained pure maltodextrin is it still a 3 FP or higher now that it has pure Maltodetxrin? Unfortunately I’m new to this and couldn’t work it out properly
Hi Norm any thoughts on this? Is unsweetened absorb plus still a 3 FP ?
Hi Michael, If it’s maltodextrin, it’s most likely zero FP.
I lost my voice due to misdiagnosed Acid Reflux that was initially caused by my Brita water pitcher. I had forgotten to change my filter and for 2 months I drank bacteria contaminated water. To make it worse I had no symptoms to let me know what the problem was. Took 5 different doctors to properly diagnose the acid reflux. But they still weren’t dealing with the source and my speaking voice was not improving. I started taking the FTD and got the app to help with food. My daily FP is around 10 and I stopped taking the prescribed PPI’s. My voice is slowly coming back but at a snails pace. I realize that after 5 months of no voice that any progress is good but how long until my voice returns? Will anything help it recover quicker?
Hi Norm, I honestly cannot believe that doctors don’t have or just won’t promote this information!! I too was prescribed PPIs after a diagnosis of Barrett’s which were no help at all. I also have all the symptoms of LPR although my GI didn’t seem to really know about the issue to diagnose it. Nonetheless, I can’t wait to read your book, I hope to be able to get it soon.
I’d like to know, why is it that everyone I know eats as much or more carbs and sugar than I do but they’ve never had any problems. And in addition, I am already getting depressed and feeling sorry for myself that I’ll have to give up most carbs, especially sugar, can one expect to eventually have balance restored and go back to a typical diet(as otherwise unhealthy as it may be!)? I Love Sweets!!
Another question when you get around to me, are you familiar with the “30 Day Heartburn Solution” by Craig Fear? I understand that he also blames imbalance in the gut for heartburn and has great success and reviews. I have decided to go with your book but was wondering if you know how his solution compares.
Hi Michael,
A couple of quick points. Not everyone can tolerate more carbs. Look at the numbers. IBS – 50 million people, Heartburn 60 million people, SIBO related – well over 100 million people. You can still have sweets, but follow the recommendations in the book.
As for Craig Fear’s book, I don’t think it’s appropriate for me to comment.
I understand, thanks for the reply!
Have sprouted grains and beans been calculated for fermentation potential? Thank you. Marion
I can only to,state cooked fruits. Does this change the calculation? Thanks. Marion
Correction to previous comment. It shpuld have stated I can only tolerate cooked fruits. Does this change the calculation? Thanks. Marion
Hi Norm! In your IBS Fast Tract Book, pg. 73, you mention that drugs (such as Neomycin), as well as SIBO, intestinal infections, or inflammation can damage the brush border in areas of the duodenum and jejunum. I have been working on ridding myself of SIBO, methane dominant, for years. Recently reading your book. I have tried 3 regimens over the past 3-4 years, one just Rifaximin, one Rifaximin and a flagyl, and one with Rifaximin & Neomycin, which of course is preferred for methane dominance. I am trying your diet, however, believe I may need the Neomycin, as I may have had SIBO for decades. Wondering where your research is from regarding the Neomycin being damaging? Thank you so much; your book has been very informative.
Hey Donna, Thanks for reading and I hear you. Taking antibiotics is not without risk, especially for those absorbed systemically. Yes, there is some work showing neomycin-related mucosal damage, though how much is drug-related and how much is related to changes in gut bacteria, was not resolved here. Here is a link. https://bit.ly/2jxN1UK
This study, though in mice, suggests the effects my be more drug related since they differ from germ-free mice. https://bit.ly/2ktAcLr
Here are a couple more refs on this:
https://bit.ly/2jxULpP
https://bit.ly/2jSdVHP (may need to get if from library)
But I would be more concerned with this quote from https://www.drugs.com/sfx/neomycin-side-effects.html “Since oral neomycin is absorbed systemically after oral administration, its use may result in nephrotoxicity, neurotoxicity and/or ototoxicity, even at recommended doses and in patients with normal renal function”
Hello, what is your advise for the best type/lowest FP of cream or milk to add to my morning coffee? I have been using Nestle Coffee-Mate Bliss, flavor: sweet cream…. I think it’s FP value is way too high, and need a good alternative please. I also use 1 packet of Natra-Taste sweetener in my morning coffee, which I think is acceptable. Thanks for your advise and great information!
Hello Norm! How do you take into account a food that has an equal amount of fructose and glucose? Since the glucose seems to aid in absorption of foods that have fructose. How do you take into account the naturally occurring polyols found in whole foods? You mention that sugar alcohols/sweeteners are an issue, but what about in foods? (mushrooms, sweet potatoes, avocado, etc) THANK YOU very much for your work. I would love to see Recipes incorporated into your app and pictures of the foods (fruits and veggies especially so we know what they are).
Hi Norm,
I am curious about the information I read that resistant starch feeds good bacteria in the gut. Since resistant starch is a trigger for LPR, and a no-no for SIBO sufferers, it seems difficult to know what to do. Feed the good bacteria and balance the gut in hopes of resolving theunderlying issue ot avoid the resistant starch and never get “cured”? What are your thoughts onthis?
drink a cup of fennel tea every evening and it really soothes my stomach. However, I noticed that it’s listed as high FODMAP. Does this mean that it has a high FP as well? Thank you
Has amaranth been tested? The only notation I saw was amaranth mixed with wheat flour. Thanks.
Hi Marion, There was a study that tested the GI of “Amaranth popped eaten with milk”. The GI was very high – 97. It may be worth a try (I would recommend lactose free milk or light cream) as this would result in quite a low FP. Also, mixed 50% with wheat, the GI is 76, or 10 points higher than with 75% wheat. Again suggestive of high GI and hence low FP. Here’s the reference: Chaturvedi A, Sarojini G, Nirmala G, Nirmalamma N, Satyanarayana D. Glycemic index of grain amaranth, wheat and rice in NIDDM subjects. J Plant Foods Hum Nutr 1997; 50: 171-8.
I was also wondering about pea protein? Has that been tested? I am getting tested through cyrex and am looking for protein bars that cannot be confused for gluten.
Protein regardless of the source, by definition would be zero FP.
I’m on my first week with the diet without much success. My problem is non acid reflux, is the diet also for that?
The diet is designed to stop reflux, regardless if acidic or not. I suggest giving it more time for non-acid reflux / silent reflux / LPR.
Since reading your book, I have been following your recommendations for almost 2 months. I have eliminated all High FP foods, severely limited Mid FP foods and am concentrating on Low FP intake. I never had severe GERD but it was there both in stomach pain and silent GERD. I sleep on a wedge pillow, have eliminated alcohol and coffee and have not had reflux in several years. I had an upper GI check last year and the doc said there is no evidence of Barretts but I do have a hiatal hernia. He had me on two 40mg pantoprazole, one in am and one in pm.
I wanted to ease off the meds gradually. About three weeks into your recommendations, I dropped the pm 40 mg pantoprazole and since have been feeling really great. I will have a medical check up in a few weeks and will be asking the doc if I can drop to a 20mg pantoprazole in the am as an experiment. Then my plan would be to drop the 20mg next.
I eliminated bread products for a while and find that the more “whole grain” there is the more I experience very sight GERD. Otherwise I feel fine. As far as I know I am fine with lactose but am on soy milk at present but eat cheese. My problem is colon cancer runs in my family and I try to supplement insoluble fiber. I took supplements until starting your diet and found they are mostly sugar so I stopped them. I know you are iffy on fiber supplements. What can I do to make sure my BM’s are regular? Since following your recommendations, I have become a lot less regular. I eat plenty of salads and leafy greens. I would like to eat a cereal such as a bit of all bran added (1/4 C) to my regular cereal (rice chex) but it is listed as high FP.
Am I correct that cutting the portion size in one half cuts the fermentation potential in one half as well. It’s a matter of serving size. Thanks. Marion
Absolutely correct Marion.
Does marrow broth have an fp besides spices? If you add parsnips to be in the broth do they count towards fp? Thanks. Marion
I notice people ask for fp of products. Can they all be calculated by the label.? Thanks Marion
All my problems started few years ago when I was prescribed PPIs for GERD & Hiatal Hernia. Vicious circle of SIBO, constipation, everything gets backed up causing GERD and needing more PPI. Probiotics seem to make it worse (guess adding billions of bacteria to your gut does not help even if its good bacteria). Rifaxan did not help me. My homeopathic doctor suggested Berberine and a strict no-carb diet. I lost 20 pounds and could not sustain it. And the SIBO came back. I am really hoping that the diet will help. I bought the books and the app.
What do you think of Berberine? and when should I start taking probiotics again?
Yes, parsnips FPs will need to be added. Marrow broth itself has zero FP. Also yes, FPs for various products can be calculated based on their nutritional facts and GI. If no GI available use 50.
Sometimes people ask about fp of a product. Can all products be calculated with the fp calculator?
Does the fp of Jasmine rice change if it is cooked overnight in a crockpot alone or in a soup? Is it just the cooling process that creates resistant starch? Thanks. Marion
Can you help clarify which is a sweet potato and which is a yam. My grocery store is now calling orange fleshy vegetable a yam as well as the white ones. Big fp difference. I thought the orange meant it was a sweet potato. Thanks. Marion
Thank you for your comment on the FP for vanilla Absorb Plus. I am using the chocolate flavor or was until I calculated the FP on the app…..something wild like 32 points which is too high for “snack”.
Could you look at this calculation for accuracy?
Total carb…..58
Dietary fiber….2 g
Sugars….13 g
Index not noted on label
Thank you so much for all….loved the podcast with Rebecca Coombs!
Most of the carbs in this product are quick to absorb Anni. I estimate an FP of approximately 6-8. Not too terrible, but could be an issue for someone trying to stick to 20 points a day.
Thanks for tuning in for the podcast. I really enjoyed getting to know Rebecca and hearing about her amazing story.
Hi there, I have acid reflux which flares up from time to time but since following the Fast Tract Diet it has been much improved. I have had three gastroenteroscopy examinations over the years, the one in 2011 and 2014 showed I had a hiatal hernia, but since following the fast tract diet there was no evidence of a hiatal hernia at my last gastroenteroscopy in summer 2016 so am I delighted by that as I thought that once you had been diagnosed with a hiatal hernia it was irreversible – my consultant could notreally give me much of an explanation as to why this has happened but did take down details of the Fast Tract diet. I would welcome any advice as to whether Food Grown supplements may not be good for SIBO – I take a multi-supplement for general health reasons from a reputable company (Wild Nutrition) who pride themselves on their supplements being ‘food grown’. however I am detecting a potential link between a flare up of acid reflux symptoms and taking this supplement as a few times when I stopped them my symptoms seemed to calm down – however it is often difficult to pinpoint specifically what triggers a flare up so any information on ‘food grown’ supplements and acid reflux would be appreciated
Hello. Are there particular carbs on the diet to avoid with klebseilla? Thanks. Marion
I bought millet flour because the fp was low. The bag says 22 carbs, 1.5 fiber and 0 sugar. And comes out high with the calculator? Can you help me resolve my understanding of millet flour fp. Thanks. Marion
Hi Marion, The problem is likely not adjusting the glycemic value to 100 for Millet bread. See the slider at the bottom? Move that from the default (50) to 100.
Thank you so much for the reply. It does come out low. Can you explain about adjusting the glycemic index on the calculator? I tried this same thing with rice and oat flour and do not undstand glycemic index adjustment. Thanks. Marion
Do I need to adjust the glycemic index for rice and oat flour? How do I know when to change the glycemic index? Thanks. Marion
Absolutely Marion. Setting the GI is important for higher carb foods where the GI can greatly impact the FP. If you can’t find the GI in the mobile app, book, or on line (glycemicindex.com), you may need to use 50 as a conservative estimate. Since most starch foods range in GI from 45 – greater than 90, this will overestimate the FP in most cases. Then follow the pro-digestion strategies in the book and use your symptoms as a guide. To be on the safe side, you may choose only to consume starches with known GIs and hence well defined FP values.
For lower carb foods, the GI value matters much less since there are fewer carbs meaning the FP is less influenced by GI.
Hello, I just bought your book with great hope it will help, I’m waiting for it to arrive. Do you think it will help with silent re flux? I have vapors going into my lungs and it makes me cough and irritates my throat. The last couple of days I have limited my meals to green veggies, chicken and packaged turkey. My symptoms are still present. I really want this to work, my next step would be surgery. Do you know if anyone else has had these symptoms and over came them with the Fast Tract Diet?
Thank you Sue
Many people report significant progress over time on the diet. I recommend reading the Amazon reviews and connecting with other LPR folks with their stories and progress by joining the Fast Tract Diet Official Facebook group. You will need to give it some time. Read the book including the underlying causes chapter and all the trouble-shooting sections in both the book and the mobile Fast Tract Diet app.
Hello,
I am dealing with reflux (non-medicated) and IBS. I have the Fast Tract App and was using it for reflux, however, I have been getting some advice about an IBS diet from my doctor. My questions:
1. The FODMAP diet has been advised for me. There seems to be some cross-over, however, some things do not. Do you have a combination diet for IBS and Reflux?
2. Relating to 1. above. The most ‘conflict’ comes from the types of breads, grains and cereals. My GI doc calls white pastas, breads, etc “SAFE FOODS” and not to limit these. Brown rice, grain breads are to be avoided.
3. What about Fiber? I have been advised to take 1 tbsp of pysillium husk (soluble fiber) two times per day. I understand that the fast tract reduces fiber significantly. FODMAP is fine with OATMEAL.
I would appreciate your thoughts and some clarity on this. I plan to set up a virtual consultation with you as well.
Thanks
Hi Bruno, If you click on the “more” box icon on the bottom right of the screen in the mobile app (iphone, or question mark on android), you will sill see the “more” menu. Click on Fast Tract Diet, then click “read more” you will see all the chapters which explain the diet, the premise, troubleshooting, etc and how this diet is unique using the glycemic index to measure fermentable carbs (fermentation potential). Fiber, resistant starch, lactose, fructose and sugar alcohols (except erythritol) all have fermentation potential and should be limited while on the FTD. Resistant starch and fiber limitation is not part of the FODMAP diet. The evidence for limiting RS and fiber is presented clearly in both the FTD IBS and FTD Heartburn books.
Hi Norm,
Thank for your wonderful book and app and all of the research and time you’ve put into these resources. I have a couple of questions regarding discrepancies between the book and the app. As a digestive health coach and someone who’s dealt with SIBO, I want to make sure I use the correct numbers.
Here are a few examples:
Acorn squash
– book = 5 FP
– app = 8 FP raw, 16 FP cooked
Butternut squash
– book = 7 FP
– app = 9 FP raw, 14 FP cooked
Carrots, raw
– book = 7 FP
– app = 11 FP
Is the app a more accurate tool to use since it’s newer? Just want to make sure I’m advising my clients correctly. I’m going to give this protocol a try as well, so I can compare it to SCD and Low FODMAPS. The science behind your program really makes sense to me. Thanks!
Jen
Hi Jen,
I recommend carefully checking the serving sizes as that can affect the FP. Since the app focuses first on physical serving sizes, this is likely the most significant source of differences. If you see different FPs for the same serving size, please let me know and I will look into it.
Thanks,
Norm
Hello Norm! I just purchased your book and am eager to get started. Quick question. If one suspects they might have food intolerances (tenuously in my case), do you recommend eliminating these suspected foods in addition to what is eliminated on your plan? Or is there a good chance these issues will resolve on their own with the Fast Tract Diet? What would be a good strategy here? Thanks! Robin
P.S. I should note that my suspected issue is histamine intolerance, which is a bit more complex and requires eliminating lots of foods.
Food elimination based on antibody testing did not work for IBS according to 2004 UK study. And a recent study showed that limiting fermentable carbs resulted in dramatic decreases in histamine in the gut. That suggests to me that it makes sense to get on the FTD first and then see how you feel. When I have a moment I can post the refs, but they are available elsewhere in my writings as well.
That makes a lot of sense actually. Unless I don’t actually have any dysbiosis and only have histamine intolerance, but it I’m guessing that’s rather unlikely. Thanks for the quick response.
Question: I’ve just been diagnosed with both GERD, with biopsies testing positive for Barrett’s esophagus, and Mixed IBS. Lucky me! I’m pretty sure it has to do with the fact that I’ve had four separate courses of antibiotics over the last two years, mostly for dental surgeries. Do I need to buy both books? The diet is the same, correct? And I already know I have both conditions.
Hi Lori, Thanks for this question. You are correct, both books employ the Fast Tract Diet. I recommend you get the the Heartburn version. Getting on the FTD and being sure to read the underlying causes chapter as well as the trouble-shooting sections will address both acid reflux and IBS-related symptoms.
Thank you so much for the quick response! I will try it. I want to not only get rid of my GERD and IBS symptoms but hopefully heal my esophagus and reverse the Barrett’s before my follow-up endoscopy in a year, because I researched Barrett’s online after my diagnosis and it scares me to death.
I just received your book in the mail and read all of it. I am almost 100% sure I have LPR and low acid. I am 21 days off of Omeprozole. No acid rebound as I went on a strict diet 1 week prior to reducing from 40mg/day to 20mg/day. My question: what is the FP of Cow’s milk (grass-fed) Kefir and Goat’s Milk Kefir? Not sure if it’s closer to milk FP or yogurt FP.
I am hoping your book/diet will work for me in healing. Everything in your book makes sense.
Thanks so much,
Becky D.
Hi Becky and pleased to hear about your progress. The mobile app lists several commercial kefirs. If not sweetened, both types of kefir you mention should be about 4 FP per one half cup.
Thank you so much, Dr. Robillard. Yes, the Kefir is un-sweetened/plain.
Hello,
I just finished reading your book FTD. I plan to give this eating strategy a shot as I’ve been suffering from LPR for the past several years. I’ve tried all sorts of natural remedies (DGL, aloe vera juice, raw honey, ACV) but with no permanent relief. HOpefully eating a low and specific carb diet will do the trick.I have few questions for you:
1) I lift weights and feel that carbs are an essential fuel for muscle building. Would following a low FP diet impede muscle gains?
2) Are the FP numbers contingent to serving size? In other words, for example, if rice noodles have an FP of 11 per half cup, would this mean it would have an FP of 22 for one cup?
3) As part of my eating strategy – weightlifters enjoy ‘splurge’ meals. This means, once a week, I will have a splurge meal with a dessert. Would you suppose that ‘letting go’ for one meal a week would reverse all healing processes?
4) If – by following the strategies laid in the book – a person feel he/she has been cured, can they resume ‘normal’ eating again?
Thank you for your time
This is great information, but I did not see anyone pose a question about other health benefits. Will the fast tract diet help with my high cholesterol and high blood pressure?
Thanks
FTD is a lower carb diet which is generally good for both blood pressure and cholesterol.
Thank you…read your book this weekend, will begin fast tract diet tomorrow. Have been taking PPI’s for almost 20 years.
I have an inflamed gallbladder (hyperkinetic, with a HIDA score of 99%), GERD symptoms, and lost 15 pounds in one month. It started with 2 weeks of diarrhea and now my bowels are better but I have zero appetite and extreme fatigue. A CT scan of my pancreas and other organs came back clear. I am scheduled for an endoscopy to see what is going on. My question is: could my symptoms be a result of a parasite? And, if so, would your program help with that?
Hi Jen, I can’t make that assessment based on limited info. But you can certainly get a stool test to determine if you are infected with a parasite and if positive get a prescription to kill it. If you still have symptoms, our program would be worth pursuing.
Due to time constraints, I cook white jasmine rice in large batches with other ingredients added (tahini and tamari). I realize that freshly-cooked is the gold standard, but that’s not practical for me. QUESTION: In terms of the DEGREE of formation of resistant starch, does it make any difference whether the rice-casserole is kept MOIST, versus being allowed to dry out during the cooling process? Thank you!
I find your books, website, and web videos so helpful in explaining really what is going on. Thank you.
In a recent interview with Dr. Michele, I heard you say that the food causing the SIBO symptoms may have been consumed many hours before (or even yesterday).
This is is exactly why I am having so much difficulty in discovering my response to foods. I have been having almost nightly interruptions in my sleep. I will wake up 1-5 (but, usually 2-3) hours after I have gone to sleep with volumes of gas. I have to stay up 1-2 hours to burp it all up. I do not get good sleep.
How do I figure out what foods are causing my reaction? Why do some foods react quickly and others more slowly? Should I look for a specific food type depending on when my reaction occurs?
In an attempt to fix my dilemma, I have adopted a form of intermittent fasting, so I don’t eat anything after my evening meal (sometimes, as early as 4pm), just to avoid being awakened in the middle of the night. (I go to bed between 11 and 12. This obviously can be hard to do, and it doesn’t even always work. Any suggestions?
The Fast Tract Diet places heavy emphasis on eliminating fermentable carbohydrates, but it does provide some generic guidance on the ratios of fats and proteins for consumption. It’s easy to make-up for reduced carb consumption by increasing protein consumption.
Although the primary objective for this protocol is not to activate ketosis in the digestive system, could excessive protein consumption on the Fast Tract diet potentially form fermentable carbohydrates through gluconeogensis, which would then contribute to continuing symptoms?
Interesting idea PMak and you can certainly enter ketosis when you cut back carbs enough. However, I don’t think this would present much of a problem because gluconeogenisis occurs in the liver to add glucose to the blood stream, not the digestive tract.
I am using coconut cream in a can, and I am trying to figure out what the FP value is. Your app has an entry for coconut cream concentrate -1 tbsp for 2 FP. I don’t think that is the same as what I have, and that it must have some carbs and fiber in it.
The one I have – Let’s Do Organic, Organic Heavy Coconut Cream. Only has 2 ingredients – organic coconut and filtered water. The label says 1 tbsp has 4.5 gms of fat, less than 1 Gm of total carbs, with zero dietary fiber and sugars. 40 out of the 45 calories are from fat. Since this product is almost entirely fat it seems like it should have an FP of zero, or maybe 1. Am I wrong?
I couldn’t find a GI number for coconut cream, in order to calculate the FP myself. I tried.
You’re absolutely right Mallen. Less than 1 gram FP.
Great! Thank you.
Recently diagnosed with SIBO. Stayed off all carbs for the first week and doing aok..Just received and am enjoying the FAST TRACK DIGESTION book. I am reviewing grocery list items and am reviewing protein powders. Your thoughts on SunWarrior Classic please? .Here is the profile for the vanilla. Chocolate would be my first choice if possible!
Ingredients-Organic whole grain brown rice protein, rice oligodextrin, vanilla extract, stevia extract, xanthan gum, ancient sea salt, pectin.
Calories 80
Total Carbohydrate 4 g 1%
Dietary Fiber 2 g 7%
Total 1 g
Incl. Added Sugars 0 g 0%
Protein 15 g 30%
Calcium 60 mg 5%
Iron 2 mg 11%
Sodium 55 mg 2%
Most appreciative!
Hi Lynn, It’s approximately 3 FP points. Have you tried the calculator on this site and in the mobile app?
Getting there!! Been mostly reading everything I can get my hands on as it has been overwhelming. I do plan to get the app. Most appreciative of your prompt response!!
Hi, I have been using the app for about 2 months now and it really has helped my sibo symptoms. The only thing I am battling with is increasing constipation issues (something I have never had before). Are the effective ways to deal with this without disrespecting the diet? Thanks!
Hi Dave, This article includes some tips for constipation
Just one more question on the constipation/fiber issue, I see that Psyllium Husk fiber (Now Foods) is ok (4FP teaspoon). But I was told Psyllium is a major source of soluble fiber and therefore also a strong prebiotic and not a good idea in case of SIBO. What is your opinion on this? Thanks!
Hi there. I bought the book quite some time ago, but I have a question that is not really answered in it.
Juices. So I use an extractor and make juices from apples, carrots, etc. Of course it removes all the fiber.
So is this still problematic and fermentable? The low fodmap diet I believe says fruit juices can be a problem but I want your opinion. Juices/Liquids empty through the stomach very rapidly correct?, its liquid after all and higher GI without the fiber. So would the bacteria still feed and multiply on it?, if so, what would they be feeding on?(if not the fiber), just the simple sugar components?(which should have less FP than if it had the fiber with it)
Hi San, Most juicers remove some of the insoluble fiber which would be expected to reduce the FP, while leaving all of the soluble fiber. Since I don’t know exactly how much of a reduction this is, we recommend people add up the FP values for all veggies and fruits used as the most conservative approach.
Norm, Does juice not bypass the small intestine?
Tell me another thing about GI. The book says a high GI Roll is fine and quickly digested, but how is this possible?. How is it “quickly” digested?. Even still, the wheat would still contain the fodmaps, no?.
The GI is a measurement of how quickly the carbohydrates in a food enter the blood stream relative to glucose. Wheat does contain some fodmaps, but a relatively small amount – 1- 3%.
On the Fast Tract app, it says that brown rice pasta has a 3 FP rating while virtually all of the other pastas are much higher or in double figures. Can you please confirm that the rating for brown rice pasta is correct? If not, what is the correct FP for brown rice pasta?
Hi Jallen, That is correct. It does have a lower FP due to a higher glycemic index compared to other wheat-based and bean-based pastas.
Could you help explain this? https://pubs.acs.org/doi/abs/10.1021/jf950824d?journalCode=jafcau . Does steaming increase resistant starch according to them?. Also, I did research and baking has higher resistant starch than boiling when it comes to potatoes. Something to add to your next book.
Hi,
Does the process of soaking nuts (and then low-temperature dehydrating them), which I understand makes the nutrients in nuts more available to the body, make any difference to their fermentation potential and so lower the FP?
Thank you
I read a study not too long ago that showed that soaking beans reduced the fiber content (stachyose and otehrs) by approximately 25%. But tree nuts are not legumes, so not sure.
Dr Robillard:
I have a question regarding oysters. I have found out oysters, like scallops, have carbs.
Is it safe to consume oysters then?
Yes, many shellfish including oysters, mussels, abalone, whelk, clams, octopus and scallops contain some carbs (1-7%) as well as either insulin or an insulin-like substance which I find interesting. Several more have been added to the FTD mobile app – update due out in next couple of months. I have been looking into the nature of the carbohydrates in seafood. So far, I have found reports that both glucose (GI 100) and trehalose (GI 38) are present, but not sure of the ratio. Currently we estimate FP with a conservative GI of 50. I’m interested in learning more about the nature of these carbs. Let me know if you find any info on this.
As for your question, I see shellfish as a healthy nutrient dense food. I don’t see the few carbs as a big problem, especially if you include the FP points in your daily allowance.
I have recently bought your book and am using your fabulous app. I am a bit confused however the app uses 20 as the maximum low range we should target daily and your book says 30. Which should I use?
Hi sspect, Yes, feedback from people using the diet convinced us that lower daily FP points are needed at times for challenging symptoms. Also, cutting back on low FP carbs as mentioned in the troubleshooting sections may also be needed at times with problematic digestion. Many people go to 15 or even 10 periodically to control symptoms, especially early on.
As I navigate thru the first week of recipes I have some questions. For the past five years my husband and I have moved our diet to a whole food, plant based diet. We have worked hard on this change and are proud of our commitment. However, since most of your menu selections are more paleo in nature I am feeling a bit overwhelmed and lost in how to complete Fast Track diet and honor my core values of not eating animal products. How do you support whole food, plant based patients with this dilemma? I have been able to compromised in making at least homemade yogurt but do not want to consume more animal products. Can I continue to use my coconut hemp milk even if it has Gellan Gum? By the way, I am very impressed with the speed in which you answer questions … perhaps in the future a Fast Track Plant Based book could be included in your offerings. No small request – I am sure.
So it seems that for many of us who think we’re suffering from GERD, but actually have SIBO, one of the benefits (along with reducing intergastric pressure) of following the Fast Tract diet is that it reduces/stops the very painful inflammatory response in the gut in reaction to the bacteria. So I’m therefore confused why your diet sometimes recommends “bad fat” foods like wings, since these kinds of fats have also been shown to cause an inflammatory response in the gut. I’d love it if you could shed light on this. Thanks!
I understand that fats have been blamed for everything from gut inflammation to high cholesterol and cardiovascular disease. But a new generation of scientists are questioning these ideas and concluding that the real culprit is a high carbohydrate diet leading to dangerous insulin levels. I recommend watching some of Ivor Cummin’s lectures on Youtube or his website TheFatEmperor.com.
Hi Norm,
In your FP calculation system it is my understanding that no matter the dose both pure glucose and jasmin rice have a FP value of zero.
Yet the most validated breath test for SIBO uses glucose and counts on it fermenting in the small intestine. So at least in some people with SIBO, glucose can ferment. How does this fit with your system and recommendations?
Bonus question: If one has been tested for lactose tolerance and have no issues – can it be assumed lactose/milk products to have a FP of zero for that person?
If I have misunderstood the fast tract FP system please clarify for me.
Thank you
Hi Fred,
Great observations. The FP calculation is based on the glycemic index (GI) and nutrition facts. It’s a great way to compare different foods and indicates that glucose is rapidly absorbed in the small intestine as is jasmine rice and certain other carbs in relative terms. However, it is important to keep in mind that the GI is determined in “10 healthy volunteers”. You might imagine that the GI of carbs such as glucose and jasmine rice might be lower (and hence “effective” FP higher) if determined in people with say, SIBO, celiac disease or other malabsorption issues. For this reason the FTD trouble-shooting tips include reducing even simple low FP carbs for a period if symptoms are not resolving.
Given this limitation, it still makes sense to choose lower FP carbs over those with high FP, but overall carbohydrate reduction is also a part of the strategy and why the recommended serving sizes of low FP carbs such as jasmine rice are relatively small, 1/2 cup in this case.
Also, good point about lactose. If you are tested and found to fully digest and absorb lactose (lactose tolerant), you can assume lactose for you has a low FP. The reason lactose has a low GI likely reflects the high prevalence of lactose intolerance in the general population.
Thank you for the quick reply Norm.
In light of your answer, does it make sense to test your own glycemic response to some foods, in order to determine the speed of absorption in one’s own specific case?
I can’t help but think that some of the factors that determine the glycemic response are not related to absorption, such as protein intake promoting insulin release and thus blunting blood glucose elevation, or even well absorbed fructose not being measured as glucose in the blood.
Dr. Norm, Is it true that eating eggs feed your bad bacteria? Dr.Roizen/Dr.Oz are saying that the choline in eggs are bad for the gut?. I eat one egg every day! Please tell me what you think, Thank You..
Hi Christine, Not sure what source info these Drs are referring to, but choline is an essential nutrient. https://www.ncbi.nlm.nih.gov/pubmed/2010061
I noticed watermelon is high FODMAP yeah according to your fermentation profile it’s low. Also most soya milk in the UK has as a high amount of oligosaccharides in surely that would make it high FP??
Hi Davies,
The FTD is a different system from FODMAP. FTD is quantitative – not “all or nothing”. It depends on the glycemic index and carbs, fiber and added sugar alcohols. In the case of watermelon, yes it has some sucrose and fructose, but according to the glycemic index most of the sugars are absorbed relatively quickly, so it has a comparatively low FP. Could certain individuals have a problem with watermelon, sure. But the FP is designed to compare it to the digestibility of other foods. The same applies to soy milk. Regular milk also has oligosaccharides too. And you will notice that even lactose-free milk has some FP points reflecting this.
My daughter just started the FAST TRACT diet—my question is do the points vary at all base on weight? My daughter is a very petite 23 year old (about 100 pounds)–would she be allowed the same number of fermentation points as a man who is 6 foot tall and weighs 225 pounds? Or would the same amount of gas produced affect her worse because she is in a tiny body?–necessitating her to be more restrictive than the average?
Great point Sara,
It does matter.Larger people can get away with more points. At 100 lbs, you would expect to eat less food and proportionally fewer points.
I have had gastroparesis for over 20 years with only occasional flareups. My flareups normally last 1 to 3 days so no big deal. However, I had the flareup from hell that lasted for 20 weeks after having a bacterial gastroenteritis. In addition, I now have SIBO. My gastroparesis is back to normal but I’m still dealing with the SIBO. My doctor put me on an herbal preparation in lieu of antibiotics as a more conservative measure. It did not work. I am planning on trying the Fast Track Diet still in lieu of antibiotics.
Having said all of that, when I am not in a flare I eat an extremely healthy diet and always have. The thought of never being able to eat whole grains, fruits, vegetables, peas and beans, etc. again is rather depressing. Assuming I get complete relief, if I were to start eating my normal all natural way is that going to cause the SIBO to come back?
Hi Miclew,
You might consider our consultation program where I would work with you directly to understand exactly what’s going on that is causing these episodes. On the FTD, you will find that no food is “illegal” but using the FP point system will show that many grains and legumes are high in points thus requiring some limits (smaller serving sizes or elimination) on these foods. If you are interested, please give us a call to set up a free preconsult so I can learn more about your situation and make a recommendation regarding our programs.
Do you have any thoughts about D-Ribose? It supposedly doesn’t act like a typical sugar in the body and seems to be some evidence it can improve motility, but I’ve seen it said that the glycemic index is negative, so would that be bad in this case? Thanks.
I have not investigated this sugar, but it looks really interesting (hey it’s found in meteorites!). On the one hand, in rabbits and reportedly in humans it’s thought to be absorbed quickly. However the potential GI side effects noted suggests it may not be absorbed as quickly as glucose. I have not read any papers on it’s role in motility, but please do post any studies you find on this. I will take a look.
As for the glycemic index, if it’s not quickly converted to glucose (measured in the GI test), it won’t as you said register as a positive number.
https://www.emedicinehealth.com/ribose/vitamins-supplements.htm#OtherNames
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6003283/
https://www.ncbi.nlm.nih.gov/pubmed/24272966
https://en.wikipedia.org/wiki/Ribose
https://examine.com/supplements/d-ribose/
https://www.drmyhill.co.uk/wiki/D-ribose
Thanks for the quick reply!
This is the one study I stumbled across on motility – but just an animal study.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4870713/
Also, is there a ‘time between meals’ for servings? Sometimes I like to snack in small amounts and that seems to suit the Fast Tract method. For instance I’ll have 4-5 raspberries, then wait an hour, then have some more food, etc. So my indulgences are small amounts but I might have more than 3 meals in a day (or more compressed meal periods when I’m doing intermittent fasting).
Just was wondering if there were a general ’90 minutes’ or something where you could count it as a new portion.
Thanks again!
Link does not seem to work. Adding some intermittent fasting is a great idea. But if you don’t leaving at least a 5 hr window without eating at least once per day is a good practice to allow the migrating motor complex to complete a cycle.
Hmm, not sure why the link didn’t work. How’s this?
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4870713/pdf/ijbsv12p0701.pdf
Okay great. I usually do at least 12 hours intermittent fasting, but it sounds like the rest of the day I can just space out snacking as long as my overall FP isn’t too high and that should be better than just 1 or 2 big meals – since some of your FP limits seem to be per meal in addition to per day. And that fits my anecdotal experience that larger meals can sometimes be harder to digest.
This seemed like a relatively recent study – does it have additional info on rice? It seems like the specific cultivar can even make a difference (along with cooking), but I don’t have access to most journal articles so I couldn’t see further.
https://onlinelibrary.wiley.com/doi/abs/10.1002/star.201900090
Great. Thanks
Would combining a fat and a carbohydrate in the same meal potentially change the FP and glycemic index? My understanding is combining fat with other foods lowers the GI because it delays stomach emptying. I’ve noticed that jasmine rice is fine, but it doesn’t digest quite as smoothly when I add butter. Before the Fast Tract Diet, I was eating a good amount of butter and cheese, so I don’t think a tablespoon of butter would have a drastic effect on its own.
Any thoughts on combining fats with carbs at the same meal changing FP?
Thanks!
Fats will lower the GI. But lower FP carbs are still a better choice. There is some data indicating the effect is greater with amylose starch, the more resistant form to begin with. Since jasmine has less amylose and more amylopectin, the effects should be less.
After completing a month and a half on the diet, I’m slowly adding back some foods, plus doing a trial of a more keto-based diet (so no more jasmine rice). I really like the jasmine rice, but I think it might give me more ups and downs in my energy level (which would make sense with such a high GI).
What are your thoughts on dark chocolate? I read in the book that you avoid chocolate or recommend higher GI chocolates. But once you’ve completed 4+ weeks on the diet, would smaller portions of dark chocolate (25g of 90% cocoa content) be suitable?
I’ve also turned a few people on to the book and they’ve found it very helpful.
Thanks again!
I don’t see why not haplo. Just keep some notes as symptoms from fiber can occur many hours after consuming it. Less than an ounce shouldn’t be too much trouble.
Hello Dr Norm Robillard.
I’ve had now gaestrophageal reflux disease for 2 years. It has affected my ability of sleeping, I cough much at night and it has affected even on my voice. There have been times I haven’t been able to speak because of the pain caused by making voice, my voice has been also very cracking.
I have went trough a endoscopy, where was only found that my LES has weakened. I was told to take Proton pump inhibitors, for a portion as big as 80mg per day. And I did take them twice a day for more than 6 months.
It just didn’t feel right to take these meds, when there had been so little told about the underlying cause of reflux. So I quited taking meds, even tho I had symptoms. So I began researching and found your book heartburn cured and started to follow nutritional tips you suggested.
Here’s problem’s that have occured, in wich I’d like to have some help.
I cutted down my daily carb intake to 25 net carbs per day for a week, but this didn’t help me much at all.
I increassed the ammount of daily carbs by 5, so Im eating now 30 net carbs per day, I have done this now for 3 weeks, but the symptoms of gerd don’t go away.
I still get lot of bloating, theres lot of gas produced in my stomach, wich gets out as burps or other way around. Theres still acid that arises causing pain in my chest and neck. Theres also slime that arises in my mouth.
Heres my question: If cutting down carbs to 25 net carbs per day doesn’t help me, should I consider moving to completely ketogenic diet? How much Carbs should a person like myself in my situation consume daily?
I’d also like to ask about the macronutrient ratio. How much should one consume fat, protein daily and in what ratio? Should there be less fat and more protein? Right now Im consuming 210 grams of fat and 71 grams of protein daily, (I try to gain muscle.)
I’d also like to ask what do you think about HCL as helping in food absorption? I have used HCL now for month at least before 2 meals a day, but there’s not been help on reflux by it, but on digestion it has helped tho.
Hi hejam,
I’m sorry to hear about your challenging symptoms. I recommend checking out our consultation program. I work with many people in your situation. I focus on three main areas – digestion and absorption, identifying and addressing potential underlying conditions (not guessing RE low stomach acid, etc.) and prodigestion behaviors and practices. Together, potentially with some very specific supplements this approach works to address the most important issues.
It’s nice (especially now) to store leftovers after meals. I usually freeze them right away to avoid any potential histamine build up.
For foods like potatoes and rice (regular or porridge), would freezing it and then reheating in the microwave create a large amount of resistant starch? Are other methods of reheating better to break down the resistant starch?
Thanks!
When it comes to starches, fresh is best. Refrigerated and likely freezing too can increase the amount of resistant starch. Keeping them moist wrapping it tight and reheating well should help regelatinize the starch, but not as good as fresh. Try it and limit the serving size. See how you do.
Hello Dr Norm, I would like to ask simply what vegetables I should consume to get my daily carb goals fullfilled?
I currently can only eat lettuce, spinach and zucchini.
I cannot handle cabbages, I bloat and get gerd symptoms. I wonder why? It’s hard to get daily carb goal fullfilled with only lettuce, spinach and zucchini, mentioned earlier, since they contain so little net carbs. Is there any other vegetables/low net carb vegetables I should consider using? I am also sensitive to fodmaps.
And oh my goal is to eat 20 net carbs per day. Thanks!
Regards Hejam
The diet explains the difference in freshly cooked vs cooked, cooled and reheated foods such as rice. Obviously it would be impossible to work 40 hours a week and make fresh rice every meal. Would you recommend omitting starchy foods unless only cooked fresh? I generally workout in the afternoon and then I am at work for the next 8-10 hours with no way to cook fresh foods, only microwave. (Also, adding extra fats has been difficult due to my malabsorption of them).
Small servings of well reheated moist low FP starches chewed well and eaten slowly might be Ok to try when your symptoms are more under control.
Hi there!
I was listening to some of your podcasts with other professionals about how histamine is related to SIBO. Super helpful! I think I’ve been emphasizing low histamine foods, while still massively overdoing it with fermentable carbohydrates. That said, if you suspect someone has both issues with excess histamine and SIBO, are there specific high histamine foods that you recommend they eliminate? What are the biggest problem foods or drinks in your opinion in terms of histamine? I was thinking it might be a good idea for me to follow the fast tract diet, while also eliminating the primary offenders in terms of histamine overload.
Thank you!
Hi Budgiemom, Good question. I do prepare protocols that include histamine/mast cell issues/diagnostics/foods and incorporate the FTD principles for my clients. A good place to start might be significant reduction in fermentable carbs that will greatly reduce histamine produced in the gut along with a trail of DAO or even testing for DAO levels. Also, while there are excellent AOAC test methods to measure histamine (and other amines) in food, most of the histamine data for foods is not based on this testing and often based on anecdotal reports on how someone tolerated that food which makes little sense to me.